What is a skin infection?
Your skin is the largest organ of your body. Its function is to protect your body from infection. Sometimes the skin itself becomes infected. Skin infections are caused by a wide variety of germs, and symptoms can vary from mild to serious. Mild infections may be treatable with over-the-counter medications and home remedies, whereas other infections may require medical attention. Read on to learn more about skin infections and what to do if you have one.
What are the types of skin infections?
The following are four different types of skin infections:
1. Bacterial skin infections
Bacterial skin infections often begin as small, red bumps that slowly increase in size. Some bacterial infections are mild and easily treated with topical antibiotics, but other infections require an oral antibiotic. Different types of bacterial skin infections include:
cellulitis
impetigo
boils
leprosy
2. Viral skin infections
Viral skin infections are caused by a virus. These infections range from mild to severe. Different types of viral infections include:
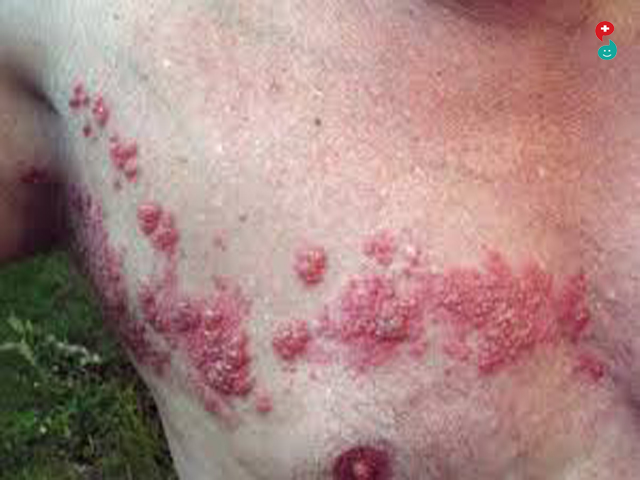
shingles (herpes zoster)
chickenpox
Molluscum contagiosum
warts
measles
hand, foot, and mouth disease
3. Fungal skin infections
These types of skin infections are caused by a fungus and are most likely to develop in damp areas of the body, such as the feet or armpit. Some fungal infections aren’t contagious, and these infections are typically non-life-threatening.
Different types of fungal infections:
athlete’s foot
yeast infection
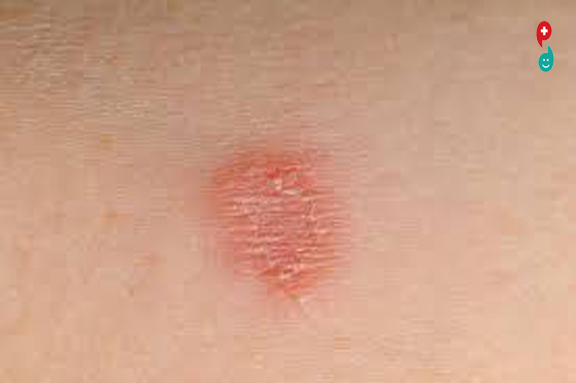
ringworm
nail fungus
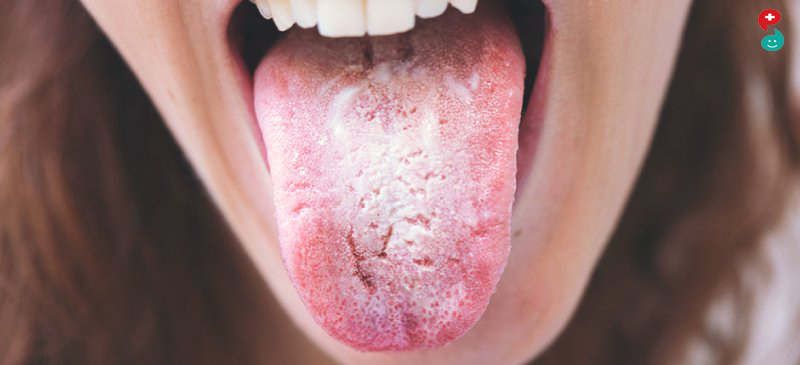
oral thrush
diaper rash
4. Parasitic skin infection
These types of skin infections are caused by a parasite. These infections can spread beyond the skin to the bloodstream and organs. A parasitic infection isn’t life-threatening but can be uncomfortable.
Different types of parasitic skin infections include:
lice
bedbugs
scabies
cutaneous larva migrans
Pictures of types of skin infections
What are the symptoms of skin infection?
The symptoms of a skin infection also vary depending on the type. Common symptoms include redness of the skin and a rash. You may also experience other symptoms, such as itching, pain, and tenderness.
See a doctor if you have pus-filled blisters or a skin infection that doesn’t improve or gets progressively worse. Skin infections can spread beyond the skin and into the bloodstream. When this happens it can become life-threatening.
Signs of a severe infection include:
pus
blisters
skin sloughing, breakdown
dark, necrotic-appearing skin, or skin that becomes discolored and painful
What are causes and risk factors for a skin infection?
The cause of a skin infection depends on the type of infection.
Bacterial skin infection: This occurs when bacteria enter the body through a break in the skin, such as a cut or a scratch. Getting a cut or scratch doesn’t necessarily mean you’ll develop a skin infection, but it does increase your risk if you have a weakened immune system.
A decreased immune system can be the result of an illness or the side effect of medication.
Viral skin infection: The most common viruses come from one of three groups of viruses: poxvirus, human papillomavirus, and herpes virus.
Fungal infection: Body chemistry and lifestyle can increase the risk of a fungal infection. For example, you may experience multiple bouts of athlete’s foot if you’re a runner or if you sweat a lot. Fungi often grow in warm, moist environments. Wearing sweaty or wet clothes is a risk factor for skin infections. A break or cut in the skin may allow bacteria to get into the deeper layers of the skin.
Parasitic skin infection: Tiny insects or organisms burrowing underneath your skin and laying eggs can cause a parasitic skin infection.
Fungal infections are common throughout much of the natural world. In humans, fungal infections occur when an invading fungus takes over an area of the body and is too much for the immune system to handle.
Fungi can live in the air, soil, water, and plants. There are also some fungi that live naturally in the human body.
Like many microbes, there are helpful fungi and harmful fungi. When harmful fungi invade the body, they can be difficult to kill, as they can survive in the environment and re-infect the person trying to get better.
In this article, we take a look at who is most at risk of getting a fungal infection and what the symptoms and treatment options are for some common types.
Symptoms
Redness and itching are common symptoms
Skin changes, redness, and itching are common symptoms of many fungal infections.
The symptoms of a fungal infection will depend on the type, but common symptoms include the following:
skin changes, including red and possibly cracking or peeling skin
itching
Read on to find out more about some common types of fungal infection, their symptoms, and the treatment options.
Types
The following conditions are all common types of fungal infections.
Athlete's foot
Tinea pedis or athlete's foot is a common fungal infection that affects the foot.
Athlete's foot is commonly associated with sports and athletes because the fungus grows perfectly in warm, moist environments, such as socks and shoes, sports equipment, and locker rooms.
In reality, anyone may be affected by athlete's foot. It is most common in warmer climates and summer months, where it can quickly multiply.
Symptoms
athletes foot
Athlete's foot is a common infection where the fungus grows in warm and moist environments.
The symptoms of athlete's foot may vary slightly from person to person. Classic symptoms include:
redness or blisters on the affected area
the infected skin may be soft, or layers may start to break down
peeling or cracking skin
the skin may scale and peel away
itching, stinging, or burning sensations in the infected area
Diagnosis, treatment, and prevention
Not all itchy feet are the result athlete's foot. Doctors usually diagnose the infection by scraping scaling skin off of a person and inspecting it under a microscope for evidence of any fungus.
There are a few different fungi that can cause athlete's foot. The infection may behave differently depending on the specific fungus that is infecting the skin.
Athlete's foot is often treated with topical antifungal ointments, which are available to purchase over-the-counter or online. Severe infections can require additional oral medications as well. The feet will also need to be cared for and kept dry to help kill the fungus.
Prevention methods include allowing the feet plenty of air to breathe and keeping them clean and dry. It is a good idea to wear sandals in public showers or locker rooms.
Yeast infection
Vaginal yeast infections are a common form of Candida overgrowth in women, usually caused by Candida albicans.
An overgrowth of Candida disrupts the normal balance of the bacteria and yeast in the vagina. This imbalance of bacteria may be due to antibiotics, stress, and hormone imbalances, or poor eating habits, among other things.
Candida infections can also commonly cause fungal toenail infections and diaper rash.
Symptoms
toenail fungus
A yeast infection may commonly cause fungal toenail infections.
Symptoms of a yeast infection include:
itching and swelling around the vagina
burning sensations or pain during urination or intercourse
redness and soreness on and surrounding the vagina
unusual vaginal discharge, such as gray clumps that resemble cottage cheese or a very watery discharge
A rash may develop over time in some cases. Yeast infections should be treated quickly, as the symptoms may become severe if left untreated.
Diagnosis, treatment, and prevention
The classic symptoms of a yeast infection make them easy to diagnose. Doctors may ask about the person's medical history, such as any previous yeast infections or sexually transmitted infections (STIs). They may also ask whether the person was recently taking antibiotics.
Doctors will then examine the vaginal walls and cervix for signs of infection, taking cells from the vagina if necessary for proper diagnosis.
Treatment of yeast infections depends on their severity. Standard treatments include creams, tablets, or suppositories, which are available via prescription, or over-the-counter or online. Complicated infections may require complex treatments.
Avoiding yeast infections begins with a balanced diet and proper hygiene. Wearing loose-fitting clothing made from natural fibers may also help prevent infection. Washing underwear in very hot water and changing feminine products often can also help prevent fungal growth.
Jock itch
Tinea cruris, commonly known as jock itch, is another common fungal skin infection.
These fungi love warm and damp environments and thrive in moist areas of the body, such as the groin, buttocks, and inner thighs. Jock itch may be more common in summer or in warm, humid areas of the world.
Jock itch is mildly contagious and is often spread through direct contact with an infected person or an object that is carrying the fungus.
Symptoms
Thrush can affect the genital area in men as well as women.
Thrush can affect the genital area in men as well as women.
Jock itch appears on the body as an itchy, red rash that often has a circular shape to it. Symptoms include:
redness in the groin, buttocks, or thighs
chafing, irritation, itching, or burning in the infected area
a red rash with a circular shape and raised edges
cracking, flaking, or dry peeling of the skin in the infected area
Cryptococcosis is caused by a fungus known as Cryptococcosis neoformans. The infection may be spread to humans through contact with pigeon droppings or unwashed raw fruit. Contact with an infected individual may also spread the infection. Individuals with disorders characterized by lowered immunity (for instance, HIV infection) are at high risk for contracting these infections.
Cryptococcosis may appear in various forms depending on how the infection is acquired. In most cases, the infection begins in the lungs (pulmonary form) and may then spread to the brain, urinary tract, skin, and/or bones (disseminated form). When the infection is limited to the lungs, symptoms may be minimal or not apparent at all. Respiratory symptoms may include coughing and chest pain. When the infection spreads, it tends to seek out the central nervous system, especially the brain. In some affected individuals, inflammation of the membranes surrounding the brain and spinal cord (meningitis) may occur as a serious complication. Symptoms associated with meningitis may include dizziness, blurred vision, severe headache, and/or stiffness of the neck. In such cases, immediate treatment is essential to help prevent potentially life-threatening complications.
Signs & Symptoms
The pulmonary forms of this disease include acute infections and chronic pulmonary infections. The disseminated forms include central nervous system (brain) infections, cutaneous (skin) infections, and infections involving other organs or systems.
Pulmonary forms.
Acute infections are only rarely diagnosed except in patients with weakened immune systems. In people with normal immune systems, cryptoccosis may not result in any symptoms at all (asymptomatic).
Chronic pulmonary infections may generate rather large masses in the lobes of the lungs, as well as segmental pneumonia (involving parts of lungs), fluid in the lungs (pleural effusions), and swollen lymph nodes.
Disseminated forms
Central nervous system infections, especially of the brain, may present as only modestly severe rather than acute. Complications may include an abnormally large head (hydrocephalus) and failing sight, among others.
Cutaneous or skin infections may present as fluid-filled bumps (papules), hardened plate-like patches (plaques), and ulcerous sores.
Infections of other organs or systems may involve sight (chorioretinitis), ears (otitis), the heart (myocarditis, endocarditis), the digestive system (gastroduodenitis, hepatitis), and the kidneys.
In general, symptoms of various forms of cryptococcosis may include: chest pain, dry cough, headache, nausea, confusion, blurred or double vision, fatigue, fever, unusual and excessive sweating at night, swollen glands without the appearance of infection in nearby areas, skin rash, pinpoint red spots (petechiae), bleeding into the skin, bruises, unintentional weight loss, appetite loss, abdominal bloating, abdominal pain, abdominal swelling, weakness, bone pain, and numbness and/or tingling.
Causes
Cryptococcosis is caused by the fungus Cyptococcus neoformans. It is spread by contact with pigeon droppings, unwashed raw fruit or by infected individuals. People with immune deficiencies or lowered immunity (such as people undergoing cancer chemotherapy or organ transplants or those infected with HIV-AIDS) are at high risk for contracting this fungal infection.
Affected Populations
Cryptococcosis occurs worldwide. In the United States it occurs predominately in the Southeastern states and usually in adults aged forty to sixty years of age. It tends to occur more often in males than females. Individuals with disorders involving reduced or impaired immunity to infection are particularly at risk.
Related Disorders
Meningitis is a possible complication of cryptococcosis. Meningitis is an inflammation of the membranes surrounding the brain and spinal cord. There are many types of Meningitis, caused by many different infectious agents with the severity of infection ranging from mild to severe.
Toxoplasmosis is an infectious disease that can be caused by contact with a microscopic parasitic organism called Toxoplasma gondii. This parasitic infection, found worldwide, can be either acquired or present at birth. The congenital type is a result of a maternal infection during pregnancy which is transmitted to the fetus, and involves lesions of the central nervous system. These lesions may lead to blindness and brain dysfunction. The disorder may be most severe when it is transmitted to the fetus during the second through the sixth month of pregnancy. Only 20% to 80% of those affected will show the presence of toxoplasmosis antibodies when tested. (For more information on this disorder, choose “Toxoplasmosis” as your search term in the Rare Disease Database.)
Diagnosis
The diagnosis depends on proof of the presence of Cyptococcus neoformans in either a bodily fluid or body tissue. The presence of the fungus may be seen under a light microscope in some circumstances; other circumstances require growing the organism from samples of fluid taken from a patient. An immunological test designed to detect the substance that would be mobilized in the body to fight this fungus if it were present (antigen) is available in commercial kits.
Standard Therapies
Treatment
Among the antibiotics used to treat cryptococcosis are the anti-fungal agents Amphotericin B, Flucytosine, and Fluconazole. These drugs may have serious side effects, so it is important for their use to be monitored carefully. Individuals with compromised immune systems, or under immune suppressive therapy, should be given prolonged drug treatment to prevent relapses.
What is Candidiasis?
There are many kinds of fungus that live in the human body. One type is called candida. It’s a type of yeast that normally lives in small amounts in places like your mouth and belly, or on your skin without causing any problems. But when the environment is right, the yeast can multiply and grow out of control.
The infection it causes is called candidiasis. There are several different types of it. Most can be easily treated with over-the-counter or prescription medications.
Thrush (Oropharyngeal Candidiasis)
When the candida yeast spreads in the mouth and throat, it can cause an infection called thrush. It’s most common in newborns, the elderly and people with weakened immune systems. Also more likely to get it are adults who:
Are being treated for cancer
Take medications like corticosteroids and wide-spectrum antibiotics
Wear dentures
Have diabetes
The symptoms include:
White or yellow patches on the tongue, lips, gums, roof of mouth, and inner cheeks
Redness or soreness in the mouth and throat
Cracking at the corners of the mouth
Pain when swallowing, if it spreads to the throat
Thrush is treated with antifungal medicines like nystatin, clotrimazole, and fluconazole. Rinsing the mouth with chlorhexidine (CHX) mouthwash may help prevent infections in people with weakened immune systems.
Genital Yeast Infection (Genital Candidiasis)
Three out of four adult women will get at least one yeast infection during their lifetime. This occurs when too much yeast grows in the vagina. (Men also can get a genital yeast infection, but it's much less common).
A yeast infection typically happens when the balance in the vagina changes. This can be caused by pregnancy, diabetes, use of some medicines, lubricants, or spermicides, or a weakened immune system. Occasionally, the infection can be passed from person to person during sex.
The symptoms include:
Extreme itchiness in the vagina
Redness and swelling of the vagina and vulva (the outer part of the female genitals)
Pain and burning when you pee
Discomfort during sex
A thick, white “cottage cheese” discharge from the vagina
A man with a yeast infection may have an itchy rash on his penis.
Because the symptoms in women can be similar to other infections like bacterial vaginosis (bacterial overgrowth in the vagina) and sexually transmitted diseases, it’s important to visit your doctor.
Most times, an over-the-counter antifungal suppository, tablet, or cream will knock out the infection. Your doctor might also prescribe a single dose of a prescription antifungal medicine like fluconazole. Tell your doctor if you get yeast infections more than four times a year. She may recommend regular doses of antifungal medication over several months to fight the repeated infections.
Diaper Rash From Yeast Infection
Though diaper rashes are usually caused by leaving a wet or soiled diaper on too long, once your baby’s skin is irritated, infection is more likely. If his diaper rash isn’t going away, check to see if his bottom is red and sensitive, and if there’s a raised red border around the sores. If so, have your pediatrician check for candidiasis. It can be treated with an antifungal cream.
Keeping your baby’s bottom clean and dry is a good start to help prevent diaper rash and candidiasis.
Invasive Candidiasis
If candida yeast enters the bloodstream (usually through medical equipment or devices), it can travel to the heart, brain, blood, eyes, and bones. This can cause a serious, life-threatening infection.
This happens most often to people who have recently been admitted to a hospital or live in a health care facility, such as a nursing home. Like other types of yeast infections, if you have diabetes, a weakened immune system, kidney failure, or are on antibiotics, your chances of getting it are greater.
The symptoms include fever and chills. Since it's likely a person with this infection is already sick with another condition, it can be hard to diagnose.
Invasive candidiasis is treated with an oral or intravenous dose of antifungal medication. If you are having surgery and have higher odds of a yeast infection, your doctor might prescribe a series of antifungal medicines before the procedure.
Overview
Athlete's foot (tinea pedis) is a fungal infection that usually begins between the toes. It commonly occurs in people whose feet have become very sweaty while confined within tight fitting shoes.
Signs and symptoms of athlete's foot include a scaly rash that usually causes itching, stinging and burning. Athlete's foot is contagious and can be spread via contaminated floors, towels or clothing.
Athlete's foot is closely related to other fungal infections such as ringworm and jock itch. It can be treated with over-the-counter anti fungal medications, but the infection often recurs. Prescription medications also are available.
Symptoms
Athlete's foot usually causes a scaly red rash. The rash typically begins in between the toes. Itching is often the worst right after you take off your shoes and socks.
Some types of athlete's foot feature blisters or ulcers. The moccasin variety of athlete's foot causes chronic dryness and scaling on the soles that extends up the side of the foot. It can be mistaken for eczema or even as dry skin.
The infection can affect one or both feet and can spread to your hand — especially if you scratch or pick at the infected parts of your feet.
When to see a doctor
If you have a rash on your foot that doesn't improve after self-treatment, see your doctor.
If you have diabetes, see your doctor if you suspect you have athlete's foot, especially if you notice any signs of a possible secondary bacterial infection such as excessive redness, swelling, drainage or fever.
Causes
Athlete's foot is caused by the same type of fungus that causes ringworm and jock itch. Damp socks and shoes and warm, humid conditions favor the organisms' growth.
Athlete's foot is contagious and can be spread by contact with an infected person or from contact with contaminated surfaces, such as towels, floors and shoes.
Risk factors
You are at higher risk of athlete's foot if you:
Are a man
Frequently wear damp socks or tight fitting shoes
Share mats, rugs, bed linens, clothes or shoes with someone who has a fungal infection
Walk barefoot in public areas where the infection can spread, such as locker rooms, saunas, swimming pools, communal baths and showers
Complications
Your athlete's foot infection can spread to other parts of your body, including:
Your hand. People who scratch or pick at the infected parts of their feet may develop a similar infection in one of their hands.
Your nails. The fungi associated with athlete's foot can also infect your toenails, a location that tends to be more resistant to treatment.
Your groin. Jock itch is often caused by the same fungus that results in athlete's foot. It's common for the infection to spread from the feet to the groin as the fungus can travel on your hands or on a towel.
Prevention
These tips can help you avoid athlete's foot or ease the symptoms if infection occurs:
Keep your feet dry, especially between your toes. Go barefoot to let your feet air out as much as possible when you're home. Dry between your toes after a bath or shower.
Change socks regularly. If your feet get very sweaty, change your socks twice a day.
Wear light, well-ventilated shoes. Avoid shoes made of synthetic material, such as vinyl or rubber.
Alternate pairs of shoes. Don't wear the same pair every day so that you give your shoes time to dry after each use.
Protect your feet in public places. Wear waterproof sandals or shoes around public pools, showers and lockers rooms.
Treat your feet. Use powder, preferably antifungal, on your feet daily.
Don't share shoes. Sharing risks spreading a fungal infection.