What is Uveitis?
Uveitis is a general term describing a group of inflammatory diseases that produces swelling and destroys eye tissues. These diseases can slightly reduce vision or lead to severe vision loss. The term “uveitis” is used because the diseases often affect a part of the eye called the uvea. Nevertheless, uveitis is not limited to the uvea. These diseases also affect the lens, retina, optic nerve, and vitreous, producing reduced vision or blindness.
Uveitis may be caused by problems or diseases occurring in the eye or it can be part of an inflammatory disease affecting other parts of the body.
It can happen at all ages and primarily affects people between 20 and 60 years old.
Uveitis can last for a short (acute) or a long (chronic) time. The severest forms of uveitis reoccur many times.
Eye care professionals may describe the disease more specifically as:
Anterior uveitis
Intermediate uveitis
Posterior uveitis
Panuveitis uveitis
Eye care professionals may also describe the disease as infectious or noninfectious uveitis.
What is the Uvea and What Parts of the Eye are Most Affected by Uveitis?
The uvea is the middle layer of the eye which contains much of the eye’s blood vessels (see diagram). This is one way that inflammatory cells can enter the eye. Located between the sclera, the eye’s white outer coat, and the inner layer of the eye, called the retina, the uvea consists of the iris, ciliary body, and choroid:
Iris: The colored circle at the front of the eye. It defines eye color, secretes nutrients to keep the lens healthy, and controls the amount of light that enters the eye by adjusting the size of the pupil.
Ciliary Body: It is located between the iris and the choroid. It helps the eye focus by controlling the shape of the lens and it provides nutrients to keep the lens healthy.
Choroid: A thin, spongy network of blood vessels, which primarily provides nutrients to the retina.
Uveitis disrupts vision by primarily causing problems with the lens, retina, optic nerve, and vitreous
What Causes Uveitis?
Uveitis is caused by inflammatory responses inside the eye. Inflammation is the body’s natural response to tissue damage, germs, or toxins. It produces swelling, redness, heat, and destroys tissues as certain white blood cells rush to the affected part of the body to contain or eliminate the insult.
Uveitis may be caused by:
An attack from the body’s own immune system (autoimmunity)
Infections or tumors occurring within the eye or in other parts of the body
Bruises to the eye
Toxins that may penetrate the eye
The disease will cause symptoms, such as decreased vision, pain, light sensitivity, and increased floaters. In many cases the cause is unknown.
What are different types of Uveitis?
Uveitis is usually classified by where it occurs in the eye.
What is Anterior Uveitis?
Anterior uveitis occurs in the front of the eye. It is the most common form of uveitis, predominantly occurring in young and middle-aged people. Many cases occur in healthy people and may only affect one eye but some are associated with rheumatologic, skin, gastrointestinal, lung and infectious diseases.
What is Intermediate Uveitis?
Intermediate uveitis is commonly seen in young adults. The center of the inflammation often appears in the vitreous (see diagram). It has been linked to several disorders including, sarcoidosis and multiple sclerosis.
What is Posterior Uveitis?
Posterior uveitis is the least common form of uveitis. It primarily occurs in the back of the eye, often involving both the retina and the choroid. It is often called choroditis or chorioretinitis. There are many infectious and non-infectious causes to posterior uveitis.
What is Pan-Uveitis?
Pan-uveitis is a term used when all three major parts of the eye are affected by inflammation. Behcet’s disease is one of the most well-known forms of pan-uveitis and it greatly damages the retina.
Intermediate, posterior, and pan-uveitis are the most severe and highly recurrent forms of uveitis. They often cause blindness if left untreated.
Diseases Associated with Uveitis:
Uveitis can be associated with many diseases including:
AIDS
Ankylosing spondylitis
Behcet’s syndrome
CMV retinitis
Herpes zoster infection
Histoplasmosis
Kawasaki disease
Multiple sclerosis
Psoriasis
Reactive arthritis
Rheumatoid arthritis
Sarcoidosis
Syphilis
Toxoplasmosis
Tuberculosis
Ulcerative colitis
Vogt Koyanagi Harada’s disease
Symptoms and Detection
What are the symptoms?
Uveitis can affect one or both eyes. Symptoms may develop rapidly and can include:
Blurred vision
Dark, floating spots in the vision (floaters)
Eye pain
Redness of the eye
Sensitivity to light (photophobia)
Anyone suffering eye pain, severe light sensitivity, and any change in vision should immediately be examined by an ophthalmologist.
The signs and symptoms of uveitis depend on the type of inflammation.
Acute anterior uveitis may occur in one or both eyes and in adults is characterized by eye pain, blurred vision, sensitivity to light, a small pupil, and redness.
Intermediate uveitis causes blurred vision and floaters. Usually it is not associated with pain.
Posterior uveitis can produce vision loss. This type of uveitis can only be detected during an eye examination.
How is uveitis detected?
Diagnosis of uveitis includes a thorough examination and the recording of the patient’s complete medical history. Laboratory tests may be done to rule out an infection or an autoimmune disorder.
A central nervous system evaluation will often be performed on patients with a subgroup of intermediate uveitis, called pars planitis, to determine whether they have multiple sclerosis which is often associated with pars planitis.
The eye exams used, include:
An Eye Chart or Visual Acuity Test: This test measures whether a patient’s vision has decreased.
A Funduscopic Exam: The pupil is widened (dilated) with eye drops and then a light is shown through with an instrument called an ophthalmoscope to noninvasively inspect the back, inside part of the eye.
Ocular Pressure: An instrument, such a tonometer or a tonopen, measures the pressure inside the eye. Drops that numb the eye may be used for this test.
A Slit Lamp Exam: A slit lamp noninvasively inspects much of the eye. It can inspect the front and back parts of the eye and some lamps may be equipped with a tonometer to measure eye pressure. A dye called fluorescein, which makes blood vessels easier to see, may be added to the eye during the examination. The dye only temporarily stains the eye.
How is Uveitis Treated?
Uveitis treatments primarily try to eliminate inflammation, alleviate pain, prevent further tissue damage, and restore any loss of vision. Treatments depend on the type of uveitis a patient displays. Some, such as using corticosteroid eye drops and injections around the eye or inside the eye, may exclusively target the eye whereas other treatments, such immunosuppressive agents taken by mouth, may be used when the disease is occurring in both eyes, particularly in the back of both eyes.
An eye care professional will usually prescribe steroidal anti-inflammatory medication that can be taken as eye drops, swallowed as a pill, injected around or into the eye, infused into the blood intravenously, or, released into the eye via a capsule that is surgically implanted inside the eye. Long-term steroid use may produce side effects such as stomach ulcers, osteoporosis (bone thinning), diabetes, cataracts, glaucoma, cardiovascular disease, weight gain, fluid retention, and Cushing’s syndrome. Usually other agents are started if it appears that patients need moderate or high doses of oral steroids for more than 3 months.
Other immunosuppressive agents that are commonly used include medications such as methotrexate, mycophenolate, azathioprine, and cyclosporine. These treatments require regular blood tests to monitor for possible side effects. In some cases, biologic response modifiers (BRM), or biologics, such as, adalimumab, infliximab, daclizumab, abatacept, and rituximab are used. These drugs target specific elements of the immune system. Some of these drugs may increase the risk of having cancer.
Eyestrain
Overview
Eyestrain is a common condition that occurs when your eyes get tired from intense use, such as while driving long distances or staring at computer screens and other digital devices.
Eyestrain can be annoying. But it usually isn't serious and goes away once you rest your eyes or take other steps to reduce your eye discomfort. In some cases, signs and symptoms of eyestrain can indicate an underlying eye condition that needs treatment.
Symptoms
Eyestrain signs and symptoms include:
Sore, tired, burning or itching eyes
Watery or dry eyes
Blurred or double vision
Headache
Sore neck, shoulders or back
Increased sensitivity to light
Difficulty concentrating
Feeling that you cannot keep your eyes open
When to see a doctor
See your doctor if self-care steps don't relieve your eyestrain.
Causes
Common causes of eyestrain include:
Looking at digital device screens
Reading without pausing to rest your eyes
Driving long distances and doing other activities involving extended focus
Being exposed to bright light or glare
Straining to see in very dim light
Having an underlying eye problem, such as dry eyes or uncorrected vision (refractive error)
Being stressed or fatigued
Being exposed to dry moving air from a fan, heating or air-conditioning system
Computer and digital device use
Extended use of computers and other digital devices is one of the most common causes of eyestrain. The American Optometric Association calls this computer vision syndrome or digital eyestrain. People who look at screens two or more hours in a row every day have the greatest risk of this condition.
Computer use strains eyes more than reading print material because people tend to:
Blink less while using computers (blinking is key to moistening the eyes)
View digital screens at less than ideal distances or angles
Use devices that have glare or reflection
Use devices with poor contrast between the text and the background
In some cases, an underlying eye problem, such as eye muscle imbalance or uncorrected vision, can cause or worsen computer eyestrain.
Some other factors that can make the condition worse include:
Glare on your screen
Poor posture
Setup of your computer workstation
Circulating air, such as from air conditioning or a nearby fan
Eye pain is a catch-all phrase to describe discomfort on, in, behind or around the eye.
The pain can be unilateral or bilateral — in other words, you can experience right eye pain, left eye pain, or the discomfort can affect both eyes. There's no evidence that right eye pain occurs more frequently than left eye pain, or vice versa.
In some cases, such as an eye injury, the cause of the pain is obvious. But often it's difficult to know why your eye hurts.
To complicate matters, the severity of eye pain does not indicate how serious the underlying cause of the discomfort is. In other words, a relatively minor problem, such as a superficial abrasion of the cornea, can be very painful. But several very serious eye conditions — including cataracts, macular degeneration, the most common type of glaucoma, a detached retina, and diabetic eye disease — cause no eye pain whatsoever.
FIND A DOCTOR: Ready to have your eyes checked? Find an eye doctor near you.
A painful eye can produce various sensations and accompanying symptoms, which can help your eye doctor determine the cause of your discomfort and prescribe the correct eye pain treatment. These include:
A sharp, stabbing sensation
Burning eyes
A dull ache
Feeling something is "in" your eye (foreign body sensation)
Eye pain also is frequently accompanied by blurred vision, redness (bloodshot eyes) and sensitivity to light.
Causes of eye pain
Here are common causes of eye pain, based on the location of the discomfort
Pain on or in your eye
Often, eye pain that feels like something is in the eye actually is caused by irritation or inflammation of the front surface of the eye, particularly the cornea.
Common causes of pain emanating from the front surface of the eye or inside the eye include:
Corneal foreign body. Not surprisingly, what often causes a foreign body sensation in the eye is an actual foreign body. Common foreign bodies that can adhere to and become embedded in the surface of the cornea include metal shavings, inorganic grit (sand, tiny stone particles), sawdust and other organic material.
The discomfort from a corneal foreign body can range from mild to severe, and typically it is most bothersome when you're blinking (since the eyelid often is rubbing across it during blinks). Blurred vision and sensitivity to light also are common.
A corneal foreign body requires urgent attention from an eye doctor, because material embedded in the cornea can quickly cause a serious eye infection.
Most corneal foreign bodies can be removed easily in the doctor's office with the proper tools. Antibacterial eye drops may be prescribed to prevent infection while the cornea heals.
Corneal abrasion. This is a scratched cornea. Although most corneal abrasions are not serious, they can be very uncomfortable and cause light sensitivity and watery eyes.
Many superficial corneal scratches heal on their own within 24 hours. But deeper abrasions can lead to a serious eye infection and even a corneal ulcer if left untreated.
Because it's often impossible to tell if eye pain is due to a minor scratch, a deep abrasion or a corneal foreign body, it's a good idea to see an eye doctor for any sharp discomfort of the eye that does not resolve very quickly, to determine the underlying cause.
Dry eyes. Another very common cause of eye discomfort is dry eyes. Usually dry eye discomfort begins more slowly and gradually than eye pain from a corneal foreign body or abrasion. Sometimes dry eyes can lead to a corneal abrasion, because there are not enough tears on the surface of the eye to keep the cornea moist and slippery.
If using lubricating eye drops significantly improves comfort, the cause of the pain is probably dry eyes. In most cases, dry eye does not require urgent attention; but your eye doctor can perform tests to determine the severity of the dryness and recommend the most effective treatment.
Other (less common) causes of anterior eye pain, or pain "in" the eye, include:
Conjunctivitis (pink eye)
Eye infections (including fungal eye infections and Acanthamoeba keratitis)
Iritis (anterior uveitis), which is inflammation of the iris
Contact lens discomfort
A very serious cause of pain in the eye is a condition called endophthalmitis (en-dahf-thal-MITE-is), which is inflammation of the interior of the eye that most often is caused by a bacterial infection. It also can occur as a rare complication of cataract surgery.
Endophthalmitis, in addition to causing eye pain, causes redness, swollen eyelids and decreased vision. If you have these symptoms after cataract surgery or other eye surgery, see your eye doctor immediately.
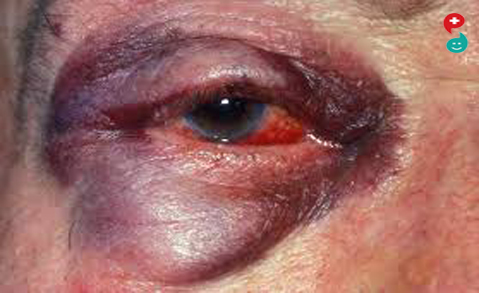
Eye injuries
Eye injuries can occur in many settings, including at home, at work or when playing sports.
Common types of eye injury include:
blows to the eye – such as being hit by a fist, elbow or ball
scratches and abrasions – such as from fingernails or tree branches
foreign bodies – such as small pieces of grit, wood or metal getting in the eye
penetrating or cutting injuries – such as cuts from glass or projectiles flung from tools, especially when hammering or using power tools
chemical burns – such as exposure to household cleaning products
radiation exposure – such as exposure to ultraviolet (UV) light from the sun or sun lamps
Wearing contact lenses incorrectly can also injure your eyes, particularly if they're dirty, don't fit properly or have been worn for too long.
What to do
Minor irritation or injury to the front of the eye usually doesn't require medical treatment and should clear up within 24 hours.
If you experience discomfort, painkillers such as paracetamol or ibuprofen may help.
Don't touch or rub your eye, apply pressure to it or wear contact lenses until it's fully healed to prevent further damage.
See your GP or optician if you have any concerns about your injury or if it's not better within 24 hours.
Flushing your eye
If you have loose particles in your eye or your eye has been exposed to chemicals, flush it out with an eyewash or plenty of clean water for at least 10 to 15 minutes. If you wear contact lenses, remember to remove them before flushing the eye.
You can flush your eyes in the following ways:
Sit down and slant your head so the injured eye is lower than the unaffected eye, ideally over a bath or sink, then use a glass or cupped hand to repeatedly pour water across the eye from the bridge of the nose.
If both eyes are affected, tilt your head back, keeping it level, and use a glass or cupped hand to repeatedly pour water across both eyes from the bridge of the nose.
If you have access to a shower, aim a gentle stream of warm water at your forehead or just above the affected eye while holding the affected eye open.
If you're working outside, you can use a garden hose to rinse your eye using a very low flow setting.
All eye injuries caused by chemical exposure should be seen by an eye doctor or nurse as soon as possible after flushing. You should also seek immediate medical advice if there are still any foreign bodies in the eye after flushing it.
Don't try to remove any objects embedded or stuck in the eye yourself, as this can damage the eye further. These should only be removed by an eye expert.
When to seek immediate medical advice
You should go immediately to your nearest accident and emergency (A&E) department if you have:
persistent or severe eye pain
foreign bodies that can't be washed out
decreased or double vision
flashing lights, spots, halos or shadows in your field of vision
blood visible in your eye
an irregularly shaped pupil (the black dot at the centre of the eye)
pain when exposed to bright light
deep cuts around your eye
your eye is sticking out of your eye socket
You should also go to A&E if your injury was caused by an object flying at speed – for example, a projectile flung from an angle grinder; a very sharp object, such as glass or a knife; or chemical exposure. Flush your eye for at least 10 to 15 minutes before going.
Burning eyes can have several possible causes, ranging from the simple to the complex, and the burning sensation can occur with or without other symptoms such as itching, eye pain, watery eyes or discharge.
Frequently, burning eyes are caused by unavoidable environmental influences, such as strong winds or high pollen counts. However, similar sensations can be symptoms of a more serious eye problem that requires medical attention. To select appropriate treatment, it's important to first establish the cause (or causes) of your burning eyes.
"Why Do My Eyes Burn?" — Causes Of Burning Eyes
Sometimes it's easy to tell what's causing an eye to burn. For example, your eyes might burn if you get chemicals in them, such as shampoo ingredients, chlorine from a swimming pool, or sunscreen. Other common irritants that can make your eyes burn include makeup, skin moisturizers, soap and cleaning products.
Woman who is rubbing her burning eyes.
Burning eyes can have many causes. A trip to the eye doctor is the best way to get relief.
Wearing contact lenses for long periods of time also can make your eyes burn.
Burning eyes also can stem from environmental irritants like smog, smoke, dust, mold, pollen or pet dander. If you are allergic to any of these substances, they are even more likely to make your eyes burn. However, even "clean" air can cause your eyes to burn, especially when it's particularly hot, cold or dry.
Although getting something in your eyes can cause them to burn, burning eyes sometimes signal a serious eye condition. For example, conditions such as ocular rosacea, dry eyes and blepharitis can cause symptoms of burning eyes.
In fact, anything that causes inflammation can create a burning sensation. Eye allergies, as well as bacterial and viral eye infections, can cause inflammation that leads to burning eyes. Even a common cold or the flu can cause eyes to burn.
In rare instances, burning eyes can be a sign of a serious sight- or life-threatening condition such as uveitis or orbital cellulitis
Often, burning eyes occur alongside other symptoms that can give your eye doctor clues about the root cause of your discomfort. For example, when burning eyes occur with itching, it may signal allergies; or if you have burning and eye discharge, this could mean an infection.
How To Get Relief From Burning Eyes
If a household product gets in your eyes and causes burning, the first thing you should do is check the product label for specific instructions. In many cases, you will be able to safely rinse your eyes to alleviate the burning sensation.
For example, children and adults often get sunscreen in their eyes during the warmer months. Though the burning or stinging may initially be significant, rinsing your eyes gently with clean water often will provide quick relief. (See sidebar below: "What to Do if You Get Sunscreen in Your Eyes.")
If you are taking an allergy medication, or any other medication that you believe is causing your eyes to burn, make sure you discuss your concerns with your doctor before discontinuing use.
Burning eyes caused by a dry eye condition usually can be relieved with frequent use of lubricating eye drops (also called artificial tears). When selecting a brand of artificial tears, consider one that is preservative-free — particularly if you plan to use the drops frequently. If your discomfort continues, let your doctor know, since there are other dry eye treatments that may be more effective and also help relieve your burning eyes.
Cool compresses gently applied over your closed eyelids also can help soothe burning eyes.
When To Call A Doctor
If your burning eyes are accompanied by pain or excessive light sensitivity, or if you have any eye discharge, blurred vision, eye floaters or flashes of light, double vision or other unexpected symptoms, contact your eye doctor right away for immediate attention.
Even if none of these additional symptoms occur, you should contact your eye doctor if your eyes continue to burn for more than a few days.
DID YOU KNOW?
What To Do If You Get Sunscreen In Your Eyes
Sunscreen is an absolute must for both children and adults to protect skin from the sun's dangerous UV rays. But these products cause more than their fair share of burning eyes.
Woman whose eye is burning because of sunscreen.
Getting sunscreen in your eyes at the beach is a common cause of burning eyes.
Although sunscreen won't usually cause any permanent damage, if you get it in your eyes it can cause significant discomfort and eye inflammation.
If you get sunscreen in your eyes, the first thing you should do is remove your contact lenses. Next, flush your eyes with a lubricating eye drop or artificial tear if you have either product handy. If not, you can use tap or fresh bottled water.
(It's important to know, though, that tap water can harbor microorganisms that can cause serious eye infections such as Acanthamoeba keratitis. So it's always a good idea to take a bottle of sterile eye wash liquid or artificial tears with you to the beach.)
Cold, wet compresses over closed eyes also help ease the sting of sunscreen in the eyes.
You can help the burning subside even quicker by frequently applying preservative-free lubricating eye drops (every 20 minutes or so) until you feel better.
Also, if you wear contact lenses, consider switching to daily disposable contacts so you can immediately replace your lenses with fresh ones if you get a pair contaminated with sunscreen.