Irritated skin can be caused by a variety of factors. These include immune system disorders, medications, and infections. When an allergen is responsible for triggering an immune system response, then it is an allergic skin condition.
Atopic Dermatitis (Eczema)
Eczema is the most common skin condition, especially in children. It affects one in five infants but only around one in fifty adults. It is now thought to be due to “leakiness” of the skin barrier, which causes it to dry out and become prone to irritation and inflammation by many environmental factors. Also, some people with eczema have a food sensitivity which can make eczema symptoms worse. In about half of patients with severe atopic dermatitis, the disease is due to the inheritance of a faulty gene in their skin called filaggrin. Unlike with urticaria (hives), the itch of eczema is not only caused by histamine so anti-histamines may not control the symptoms. Eczema is often linked with asthma, allergic rhinitis (hay fever) or food allergy. This order of progression is called the atopic march.
Allergic Contact Dermatitis
Allergic contact dermatitis occurs when your skin comes in direct contact with an allergen. For instance, if you have a nickel allergy and your skin comes in contact with jewelry made with even a very small amount of nickel, you may develop red, bumpy, scaly, itchy or swollen skin at the point of contact.
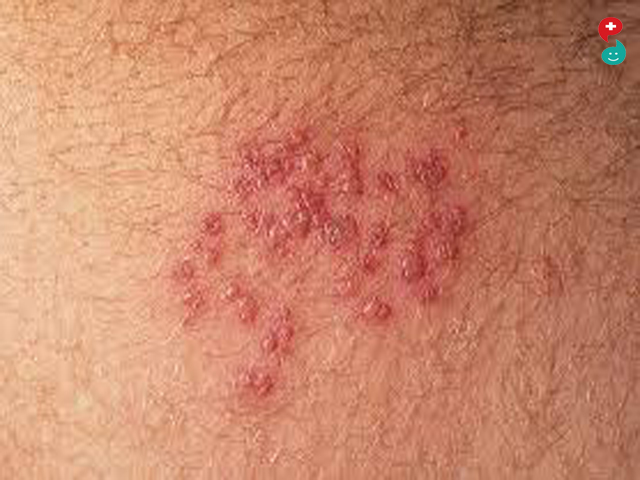
Coming in contact with poison ivy, poison oak and poison sumac can also cause allergic contact dermatitis. The red, itchy rash is caused by an oily coating covering these plants. The allergic reaction can come from actually touching them, or by touching clothing, pets or even gardening tools that have come in contact with the oil.
Urticaria (Hives)
Hives are an inflammation of the skin triggered when the immune system releases histamine. This causes small blood vessels to leak, which leads to swelling in the skin. Swelling in deep layers of the skin is called angioedema. There are two kinds of urticaria, acute and chronic. Acute urticaria occurs at times after eating a particular food or coming in contact with a particular trigger. It can also be triggered by non-allergic causes such as heat or exercise, as well as medications, foods, insect bites or infections. Chronic urticaria is rarely caused by specific triggers and so allergy tests are usually not helpful. Chronic urticaria can last for many months or years. Although they are often uncomfortable and sometimes painful, hives are not contagious.
Angioedema
Angioedema is swelling in the deep layers of the skin. It is often seen together with urticaria (hives). Angioedema many times occurs in soft tissues such as the eyelids, mouth or genitals. Angioedema is called "acute" if the condition lasts only a short time such as minutes to hours. Acute angioedema is commonly caused by an allergic reaction to medications or foods. Chronic recurrent angioedema is when the condition returns over a long period of time. It typically does not have an identifiable cause.
Hereditary angioedema (HAE)
Hereditary angioedema (HAE) is a rare, but serious genetic condition involving swelling in various body parts including the hands, feet, face, intestinal wall and airways. It does not respond to treatment with antihistamines or adrenaline so it is important to go see a specialist.
Skin conditions are one of the most common forms of allergy treated and managed by an allergist/immunologist, a physician with specialized training and expertise to accurately diagnose your condition and provide relief for your symptoms.
Deodorants and antiperspirants are items of regular use all over the world. You would never want to smell bad or have sweat stains under your armpits. Hence, after using a deodorant or an antiperspirant, you usually stick to it and keep on using it continuously. There is a major confusion regarding deodorants and antiperspirants, and it is important to know the major difference between these two similar items of everyday use.
Deodorant -
Deodorant serves the function of preventing unwanted and unpleasant odour from our body. Deodorants do not prevent sweating. Body odour is caused due to the bacterial breakdown of sweat. The ingredients of deodorant are designed especially for the elimination of the smell caused by bacteria.
The common ingredients of deodorant are :
- Water
- Sodium stearate
- Organic aloe vera juice
- Witch hazel water
- Glyceryl laurate
- Fir needle oil
- Chamomile flower aqueous extract
- Hops [CO2] extract – helps eliminate the odour
- Caprylic/capric triglyceride
- Ascorbic acid
- Silica shell
- Organic Lemongrass Oil
Antiperspirants -
Antiperspirants are different from deodorants, and they are designed in such a way that the body produces lesser sweat. This is done by blocking sweat from reaching the skin. The ingredients present in antiperspirants, especially aluminium, block the pores on the skin and do not allow sweat to pass through them. When an antiperspirant is applied to the skin, the aluminium salts get dissolved in the sweat under the armpit. The dissolved aluminium forms a gel, which acts like a plug on the sweat glands or pores on the skin. This stops sweat secretion. Aluminium is, however, a cancer-causing factor and may also lead to Alzheimer’s disease. Several forms of aluminium present in some antiperspirants leave yellow stains on clothes as a result of mixing with sweat.
The primary ingredients of antiperspirants are:
1. Aluminum Zirconium Trichlorohydrex
2. Dimethicone
3. Tribehenin
4. Artificial fragrance
5. C18 36 Acid Triglyceride
People are often confused as to what to use among deodorants and antiperspirants. This depends totally on your personal choice, but it is recommended to use a product which incorporates natural ingredients instead of using chemicals such as aluminium. Hence, deodorants are considered to be safer for everyday use. However, several artificial dyes and fragrances are used as ingredients in both deodorants and antiperspirants, which cause reactions on the skin. Allergies and skin irritation also occur sometimes as a result.
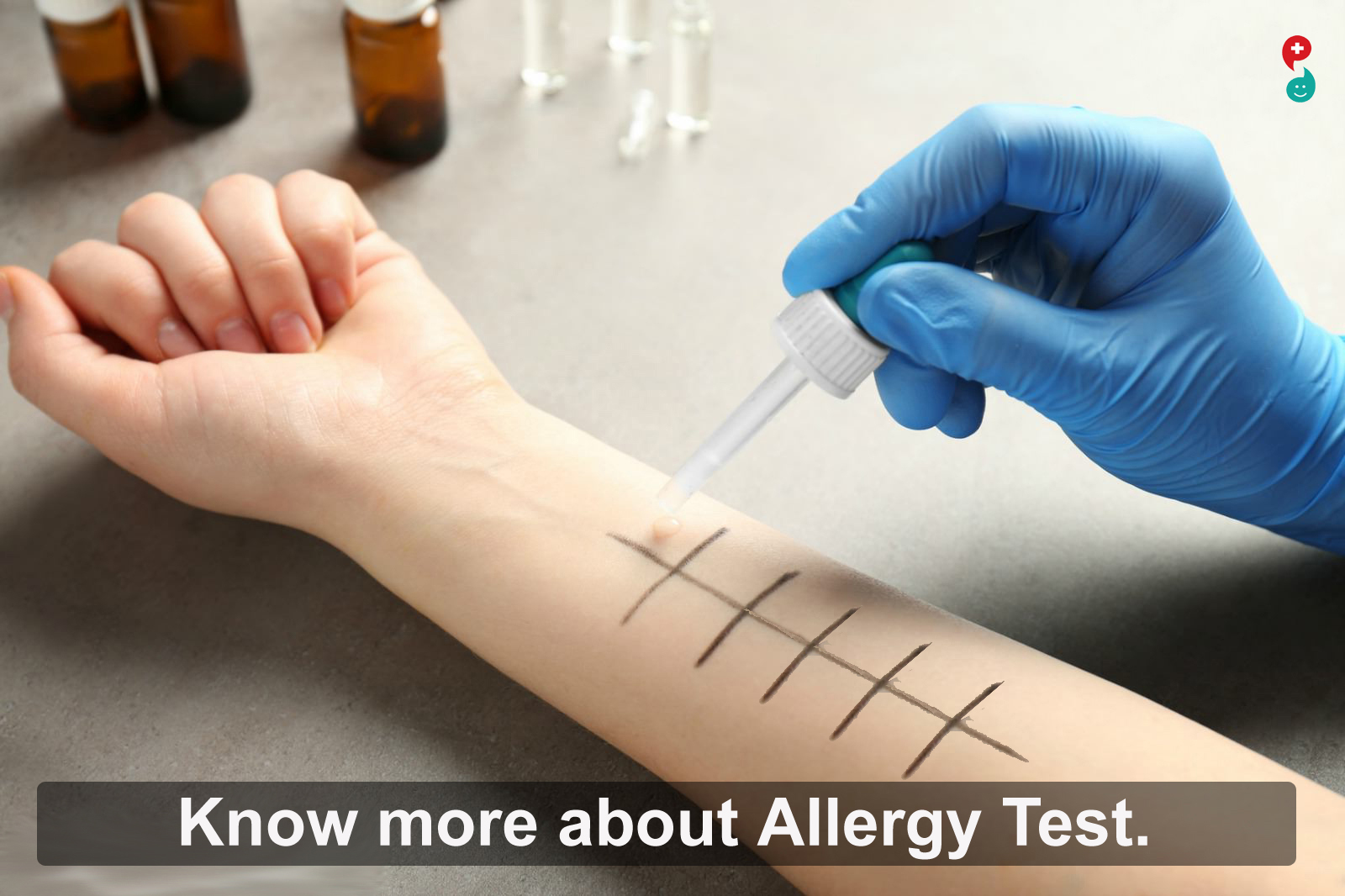
What is Allergy Test
An allergy test is an exam performed by a trained allergy specialist to determine if your body has an allergic reaction to a known substance. The exam can be in the form of a blood test, a skin test, or an elimination diet. Allergies occur when your immune system, which is your body’s natural defence, overreacts to something in your environment.For example, pollen, which is normally harmless, can cause your body to overreact.This overreaction can lead to one of more conditions like a runny nose, sneezing, blocked sinuses,itchy or watery eyes
Types of allergens
Allergens are substances that can cause an allergic reaction.There are three primary types of allergens. Inhaled allergens affect the body when they come in contact with the lungs or membranes of the nostrils or throat.Pollen is the most common inhaled allergen.Ingested allergens are present in certain foods, such as peanuts, soy, and seafood.Contact allergens must come in contact with your skin to produce a reaction.An example of a reaction from a contact allergen is the rash and itching caused by poison ivy. Allergy tests involve exposing you to a very small amount of a particular allergen and recording the reaction.
Why allergy testing is performed?
Allergies affect more than 50 million people living in the USA, according to the American College of Allergy, Asthma, and Immunology.Inhaled allergens are by far the most common type.Seasonal allergies and hay fever, which is an allergic response to pollen, affect more than 40 million Americans. The World Allergy Organization estimates that asthma is responsible for 250,000 deaths annually. These deaths can be avoided with proper allergy care, as asthma is considered an allergic disease process. Allergy testing can determine which particular pollens, moles, or other substances you’re allergic to. You may need medication to treat your allergies. Alternatively, you can try to avoid your allergy triggers.
How to prepare for allergy testing
Before your allergy test, your doctor will ask you about your lifestyle, family history, and more. They’ll most likely tell you to stop taking the medications before your allergy test because they can affect the test results. prescription and over-the-counter antihistamines, certain heartburn treatment medications, such as famotidine (Pepcid), anti-IgE monoclonal antibody asthma treatment, omalizumab (Xolair)benzodiazepines, such as diazepam (Valium) or lorazepam (Ativan)
tricyclic antidepressants, such as amitriptyline (Elavil).
How allergy testing is performed
An allergy test may involve either a skin test or a blood test. You may have to go on an elimination diet if your doctor thinks you might have a food allergy.
What is Allergy Skin tests?
Skin tests are used to identify numerous potential allergens. This includes airborne, food-related, and contact allergens. The three types of skin tests are scratch, intra-dermal, and patch tests. Your doctor will typically try a scratch test first. During this test, an allergen is placed in liquid, then that liquid is placed on a section of your skin with a special tool that lightly punctures the allergen into the skin’s surface. You’ll be closely monitored to see how your skin reacts to the foreign substance. If there’s localized redness, swelling, elevation, or itchiness of the skin over the test site, you’re allergic to that specific allergen. If the scratch test is inconclusive, your doctor may order an intra-dermal skin test. This test requires injecting a tiny amount of allergen into the dermis layer of your skin. Again, your doctor will monitor your reaction. Another form of skin test is the patch test (T.R.U.E. TEST). This involves using adhesive patches loaded with suspected allergens and placing these patches on your skin. The patches will remain on your body after you leave your doctor’s office. The patches are then reviewed at 48 hours after application and again at 72 to 96 hours after application.
What is allergy Blood tests?
If there’s a chance you’ll have a severe allergic reaction to a skin test, your doctor may call for a blood test. The blood is tested in a laboratory for the presence of antibodies that fight specific allergens. This test, called Immuno CAP, is very successful in detecting IgE antibodies to major allergens.
What is Allergy Elimination diet Test?
An elimination diet may help your doctor determine which foods are causing you to have an allergic reaction. It entails removing certain foods from your diet and later adding them back in. Your reactions will help determine which foods cause problems.
Risks of allergy testing
Allergy tests may result in mild itching, redness, and swelling of the skin. Sometimes, small bumps called wheels appear on the skin. These symptoms often clear up within hours but may last for a few days. Mild topical steroid creams can alleviate these symptoms. On rare occasions, allergy tests produce an immediate, severe allergic reaction that requires medical attention. That’s why allergy tests should be conducted in an office that has adequate medications and equipment, including epinephrine to treat anaphylaxis, which is a potentially life-threatening acute allergic reaction.
After allergy testing
Once your doctor has determined which allergens are causing your symptoms, you can work together to come up with a plan for avoiding them. Your doctor can also suggest medications that may ease your symptoms.
As complex as it may sound, Keratosis Pilaris is a harmless, non-contagious type of skin disorder, which primarily affects people with dry skin. This disease has the potential to convert a person’s once smooth skin into skin as rough as sandpaper.
Symptoms
A number of light-coloured small bumps start appearing on the skin and in most cases, they tend to appear on the upper arms, thighs and buttocks of the affected person. In certain cases, there may be some swelling or redness, which comes along with the bumps. The skin loses its original glow and colour.
Causes
As mentioned above, people with dry skin suffer from Keratosis Pilaris. Also anyone with extra sensitive skin who is prone to be allergic to various substances tend to fall prey to this disease. Often Keratosis Pilaris is inherited from other family members as well. Persons suffering from asthma and eczema have higher chances of getting affected by Keratosis Pilaris.
But what leads to such a condition? A protein in our body called ‘keratin’, which protects our skin from various infections, is the main cause behind Keratosis Pilaris. Although there is no particular reason for excess building up of keratin in our body, too much of it under the skin leads to blockages of hair follicles and growth of rashes.
Treatment
For people who are scared of medical tests, it may be a relief to know that Keratosis Pilaris does not need any sort of testing. Treatment of Keratosis Pilaris is a time taking process and immediate results may not be seen after applying a particular lotion or cream. However, sometimes it gets cured on its own without any medication.
To start off, the amount of time which is spent in water should be limited. In addition to this, there are other steps which may be taken. For example, while taking a shower, hot water should be substituted by warm water. Also, it is vital to ensure that the skin is adequately moist. Two ways of going about doing this are using moisturizers and making use of a humidifier. Make sure you use mild soaps for regular hygiene and for your shower.
Who gets Keratosis Pilaris?
Anyone can get Keratosis Pilaris. It is estimated to affect between 50-80% of all adolescents and approximately 40% of adults. Females may be more frequently affected than males. Age of onset is often within the first 10 years of life and can particularly get worse during puberty. Keratosis Pilaris may however begin at any age. A large percentage of patients have other people in their family with the same condition. It has commonly been seen in twins. Keratosis Pilaris is also seen in atopic dermatitis patients and patients with very dry skin.
One big relief when it comes to having Keratosis Pilaris is the fact that there is little risk at all if a person has it as it is not threatening. That being said, the sooner it is under control, the better!
Are you using baby wipes for your infant? If yes, then stop doing so because a new study has found that baby wipes increase the risk of developing life-threatening food allergies in children.
The genetics that alters skin absorbency, use of infant cleansing wipes that leave soap on the skin, skin exposure to allergens in dust and skin exposure to food from those providing infant care are some of the factors contributing to food allergies in babies.
Researchers said that food allergy is triggered when these factors occur together.
Joan Cook-Mills, a professor at Northwestern University in the US said,"This is a recipe for developing food allergy. It's a major advance in our understanding of how food allergy starts early in life."
Cook-Mills said that factors leading to food allergy can be modified in the home environment.
She said,"Reduce baby's skin exposure to the food allergens by washing your hands before handling the baby."
She added,"Limit use of infant wipes that leave soap on the skin. Rinse soap off with water like we used to do years ago."
Cook-Mills made the discovery by using clinical evidence about food allergy in humans, the effects of food allergen and environmental allergen exposures and neonatal mice with genetic mutations that occur in humans.
Clinical evidence shows up to 35 per cent of children with food allergies have atopic dermatitis and much of that is explained by at least three different gene mutations that reduce the skin barrier.
Cook-Mills used a neonatal mouse model with skin barrier mutations and tried exposing its skin to food allergens like peanuts. The peanuts alone had no effect.
Babies are exposed to environmental allergens in dust in a home.
"They may not be eating food allergens as a newborn, but they are getting them on their skin. Say a sibling with peanut butter on her face kisses the baby. Or a parent is preparing food with peanuts and then handles the baby," she said.
The top skin layer is made of fats, and the soap in the wipes disrupts that barrier, Cook-Mills said.
Skin problems that occur with skin barrier mutations may not be visible until long after a food allergy has already started.
The neonatal mice with the mutations had normal-appearing skin, and the dry itchy skin of dermatitis did not develop until the mice were a few months old, the equivalent of a young adult in human years.
After the neonatal mice received three to four skin exposures of food and dust allergens for 40 minutes during a two-week period, they were given egg or peanut by mouth.
The mice had allergic reactions at the site of skin exposure, allergic reactions in the intestine, and the severe allergic food reaction of anaphylaxis that is measured by decreased body temperature.
A skin barrier dysfunction was necessary for food allergy to develop in the mice, but there is a wide continuum of severe to mild skin dysfunction with eczema or atopic dermatitis, which in its mildest form may simply appear to be dry skin.
In patients with skin-barrier defects, there are changes in the proteins in the skin that are a result of mutations in the genes.
These gene mutations in patients are primarily heterozygous, which means there is a mutation in one of the two copies of a gene.
Accordingly, in the preclinical studies, neonatal mice were also heterozygous for skin barrier mutations.
The mice were co-exposed to food allergens such as egg and peanut proteins, allergens in dust (house dust mite or Alternaria alternata mold) and sodium lauryl sulphate, a soap present in infant cleansing wipes.
Cook-Mills said, these novel animal studies provide a basis to test interventions that will more effectively block the development of food allergy in infants and children.