Thrombophlebitis (throm-boe-fluh-BY-tis) is an inflammatory process that causes a blood clot to form and block one or more veins, usually in your legs. The affected vein might be near the surface of your skin (superficial thrombophlebitis) or deep within a muscle (deep vein thrombosis, or DVT). Causes include trauma, surgery or prolonged inactivity.
DVT increases your risk of serious health problems. It's usually treated with blood-thinning medications. Superficial thrombophlebitis is sometimes treated with blood-thinning medications, too.
Symptoms
Superficial thrombophlebitis signs and symptoms include:
Warmth, tenderness and pain in the affected area
Redness and swelling
Deep vein thrombosis signs and symptoms include:
Pain
Swelling
When a vein close to the surface of your skin is affected, you might see a red, hard cord just under the surface of your skin that's tender to the touch. When a deep vein in the leg is affected, your leg may become swollen, tender and painful.
When to see a doctor
See your doctor right away if you have a red, swollen or tender vein — especially if you have one or more risk factors for thrombophlebitis.
If you have leg swelling and pain and develop shortness of breath or chest pain that worsens when you breathe, go to an emergency room. These might indicate that you have a dislodged blood clot traveling through your veins to your lungs (pulmonary embolism).
Causes
The cause of thrombophlebitis is a blood clot, which can form in your blood as a result of:
An injury to a vein
An inherited blood-clotting disorder
Being immobile for long periods, such as during an injury or a hospital stay
Risk factors
Your risk of thrombophlebitis increases if you:
Are inactive for a prolonged period, either because you're confined to bed or are traveling in a car or plane for a long period
Have varicose veins, which are a common cause of superficial thrombophlebitis
Have a pacemaker or have a thin, flexible tube (catheter) in a central vein, for treatment of a medical condition, which may irritate the blood vessel wall and decrease blood flow
Are pregnant or have just given birth
Use birth control pills or hormone replacement therapy, which can make your blood more likely to clot
Have a family history of a blood-clotting disorder or a tendency to form blood clots
Have had previous episodes of thrombophlebitis
Have had a stroke
Are older than 60
Are overweight or obese
Have cancer
Smoke
If you have one or more risk factors, discuss prevention strategies with your doctor before taking long flights or road trips or if you're planning to have elective surgery, recovery from which will require you not to move much.
Complications
Complications from superficial thrombophlebitis are rare. However, if you develop DVT, the risk of serious complications increases. Complications might include:
Pulmonary embolism. If part of a deep vein clot becomes dislodged, it can travel to your lungs, where it can block an artery (embolism) and become potentially life-threatening.
Post-phlebetic syndrome. This condition, also known as post-thrombotic syndrome, can develop months or even years after you've had DVT. Post-phlebetic syndrome can cause lasting and possibly disabling pain, swelling and a feeling of heaviness in the affected leg.
Prevention
Sitting during a long flight or car ride can cause your ankles and calves to swell and increases your risk of thrombophlebitis. To help prevent a blood clot:
Take a walk. If you're flying or riding a train or bus, walk up and down the aisle once an hour or so. If you're driving, stop every hour or so and move around.
Move your legs regularly. Flex your ankles, or carefully press your feet against the floor or footrest in front of you at least 10 times each hour.
Wear loose clothing.
Drink plenty of nonalcoholic fluids to avoid dehydration.
What’s rheumatoid arthritis?
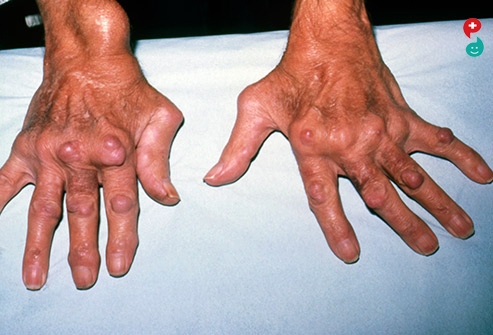
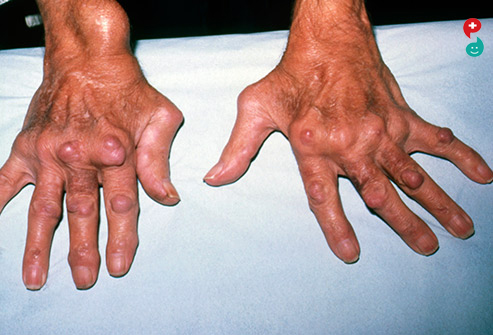
Rheumatoid arthritis (RA) is an autoimmune disease that can cause joint pain and damage throughout your body. The joint damage that RA causes usually happens on both sides of your body. So if a joint is affected in one of your arms or legs, the same joint in the other arm or leg will probably be affected, too. This is one way that doctors distinguish RA from other forms of arthritis, such as osteoarthritis (OA).
Treatments work best when RA is diagnosed early, so it’s important to learn the signs. Read on to learn everything you want to know about RA, from types and symptoms, to home remedies, diets, and other treatments.
Rheumatoid arthritis symptoms
RA is a long-term or chronic disease marked by symptoms of inflammation and pain in the joints. These symptoms and signs occur during periods known as flares. Other times are known as periods of remission — this is when symptoms dissipate completely.
RA symptoms, which can occur throughout the body, include:
joint pain
joint swelling
joint stiffness
loss of joint function
Symptoms can vary from mild to severe. It’s important not to ignore your symptoms, even if they come and go. Knowing the early signs of RA will help you and your doctor to better treat it.
Rheumatoid arthritis diagnosis
Diagnosing RA can take time and may require multiple lab tests to confirm clinical examination findings. Your doctor will use several tools to diagnose RA.
First your doctor will ask about your symptoms and medical history. They’ll also perform a physical exam of your joints. This will include looking for swelling and redness, and testing your reflexes and muscle strength. Your doctor will also touch the affected joints to check for warmth and tenderness. If they suspect RA, they’ll most likely refer you to a specialist called a rheumatologist.
Since no single test can confirm a diagnosis of RA, your doctor or rheumatologist may use several different types of tests. They may test your blood for certain substances like antibodies, or check the level of certain substances like acute phase reactants that are elevated during inflammatory conditions. These can be a sign of RA and help support the diagnosis.
They may also request certain imaging tests. Tests such as ultrasonography, x-ray exams, and magnetic resonance imaging (MRI) not only show if damage from RA has been done to your joints but also how severe the damage is. A complete evaluation and monitoring of other organ systems might be in order for some people with RA, too. Learn more about the process of diagnosing RA.
Blood test for rheumatoid arthritis
There are several types of blood tests that help your doctor or rheumatologist determine whether you have RA. These tests include:
Rheumatoid factor test: This blood test checks for a protein called rheumatoid factor. High levels of rheumatoid factor are associated with autoimmune diseases, especially RA.
Anticitrullinated protein antibody test (anti-CCP):This test looks for an antibody that’s associated with RA. People who have this antibody usually have the disease. However, not everyone with RA tests positive for this antibody.
Antinuclear antibody test: This tests your immune system to see if it’s producing antibodies. Your body may make antibodies as a response to many different types of conditions, including RA.
Erythrocyte sedimentation rate: This test helps determine the degree of inflammation in your body. The result tells your doctor whether inflammation is present. However, it doesn’t indicate the cause of the inflammation.
C-reactive protein test: A severe infection or significant inflammation anywhere in your body can trigger your liver to make C-reactive protein. High levels of this inflammatory marker are associated with RA.
Find out more about the different RA blood tests.
Rheumatoid arthritis treatment
There’s no cure for RA, but there are treatments that can help you to manage it. Treatments for RA help to manage the pain and control the inflammatory response which can in many cases result in remission. Decreasing the inflammation can also help to prevent further joint and organ damage.
Treatments may include:
medications
alternative or home remedies
dietary changes
specific types of exercise
Your doctor will work with you to determine the best types of treatments for you. For many people, these treatments can help them live an active life and reduce the risk of long-term complications. Learn more about specific RA treatments and how to treat flares.
Rheumatoid arthritis medications
There are many types of medication for RA. Some of these medications help to reduce the pain and inflammation of RA. Some help to reduce flares and limit the damage that RA does to your joints.
The following medications help reduce the pain and inflammation during RA flares:
nonsteroidal anti-inflammatory drugs (NSAIDs)
corticosteroids
acetaminophen
The following drugs work to slow the damage that RA can cause to your body:
Disease-modifying antirheumatic drugs (DMARDs): DMARDs work by blocking your body’s immune system response. This helps to slow down RA’s progression.
Biologics: These new generation DMARDs provide a targetedresponse to inflammation rather than blocking your body’s entire immune system response. They may be an effective treatment for people who don’t respond to treatment with more traditional DMARDs.
Janus kinase (JAK) inhibitors: These are a new subcategory of DMARDs that block certain immune responses. These are drugs that your doctor may use to help prevent inflammation and stop damage to your joints when DMARDs and biologics don’t work for you.
Rheumatic fever is an inflammatory disease that can develop as a complication of inadequately treated strep throat or scarlet fever. Strep throat and scarlet fever are caused by an infection with streptococcus bacteria.
Rheumatic fever is most common in 5- to 15-year-old children, though it can develop in younger children and adults. Although strep throat is common, rheumatic fever is rare in the United States and other developed countries. However, rheumatic fever remains common in many developing nations.
Rheumatic fever can cause permanent damage to the heart, including damaged heart valves and heart failure. Treatments can reduce damage from inflammation, lessen pain and other symptoms, and prevent the recurrence of rheumatic fever.
Symptoms
Rheumatic fever symptoms vary. You can have few symptoms or several, and symptoms can change during the course of the disease. The onset of rheumatic fever usually occurs about two to four weeks after a strep throat infection.
Rheumatic fever signs and symptoms — which result from inflammation in the heart, joints, skin or central nervous system — can include:
Fever
Painful and tender joints — most often in the knees, ankles, elbows and wrists
Pain in one joint that migrates to another joint
Red, hot or swollen joints
Small, painless bumps (nodules) beneath the skin
Chest pain
Heart murmur
Fatigue
Flat or slightly raised, painless rash with a ragged edge (erythema marginatum)
Jerky, uncontrollable body movements (Sydenham chorea, or St. Vitus' dance) — most often in the hands, feet and face
Outbursts of unusual behavior, such as crying or inappropriate laughing, that accompanies Sydenham chorea
When to see a doctor
Have your child see a doctor for signs or symptoms of strep throat. Proper treatment of strep can prevent rheumatic fever. Also, have your child see a doctor if he or she shows other indications of rheumatic fever.
Causes
Rheumatic fever can occur after an infection of the throat with a bacterium called group A streptococcus. Group A streptococcus infections of the throat cause strep throat or, less commonly, scarlet fever. Group A streptococcus infections of the skin or other parts of the body rarely trigger rheumatic fever.
The link between strep infection and rheumatic fever isn't clear, but it appears that the bacterium tricks the immune system. The strep bacterium contains a protein similar to one found in certain tissues of the body. So immune system cells that would normally target the bacterium may treat the body's own tissues as if they were infectious agents — particularly tissues of the heart, joints, skin and central nervous system. This immune system reaction results in inflammation.
If your child receives prompt treatment with an antibiotic to eliminate strep bacteria and takes all medication as prescribed, there's little chance of developing rheumatic fever. If your child has one or more episodes of strep throat or scarlet fever that aren't treated or not treated completely, he or she might develop rheumatic fever.
Risk factors
Factors that can increase the risk of rheumatic fever include:
Family history. Some people carry a gene or genes that might make them more likely to develop rheumatic fever.
Type of strep bacteria. Certain strains of strep bacteria are more likely to contribute to rheumatic fever than are other strains.
Environmental factors. A greater risk of rheumatic fever is associated with overcrowding, poor sanitation and other conditions that can easily result in the rapid transmission or multiple exposures to strep bacteria.
Complications
Inflammation caused by rheumatic fever can last a few weeks to several months. In some cases, the inflammation causes long-term complications.
Rheumatic heart disease is permanent damage to the heart caused by rheumatic fever. It usually occurs 10 to 20 years after the original illness. Problems are most common with the valve between the two left chambers of the heart (mitral valve), but the other valves can be affected. The damage can result in:
Valve stenosis. This narrowing of the valve decreases blood flow.
Valve regurgitation. This leak in the valve allows blood to flow in the wrong direction.
Damage to heart muscle. The inflammation associated with rheumatic fever can weaken the heart muscle, affecting its ability to pump.
Damage to the mitral valve, other heart valves or other heart tissues can cause problems with the heart later in life. Resulting conditions can include:
An irregular and chaotic beating of the upper chambers of the heart (atrial fibrillation)
An inability of the heart to pump enough blood to the body (heart failure)
Rheumatic diseases are characterized by inflammation that affects the connecting or supporting structures of the body — most commonly the joints, but also sometimes the tendons, ligaments, bones, and muscles. Some rheumatic diseases even affect the organs.
These diseases can ultimately cause loss of function in those body parts.
Rheumatic diseases include arthritis, which literally means "joint inflammation" and itself encompasses more than 100 different disorders. Rheumatic diseases that primarily affect the spine are considered spondyloarthropathies.
In all, rheumatic diseases affect more than 46 million worldwide, including 294,000 children, according to the National Institute of Arthritis and Musculoskeletal and Skin Diseases.
Types of Rheumatic Diseases
Some of the most common rheumatic diseases include:
Osteoarthritis, the most prevalent type of arthritis, which primarily affects and destroys cartilage, the soft tissue that cushions the ends of bones within joints
Rheumatoid arthritis, an autoimmune disorder in which the immune system mistakenly attacks the synovium, a soft tissue that lines the joints, leading to inflammation
Fibromyalgia, a chronic condition marked by tender points and localized pain throughout the musculoskeletal system
Systemic lupus erythematosus, or simply lupus, an autoimmune disorder that causes inflammation in numerous parts of the body, including the joints, skin, kidneys, blood, lungs, heart, and brain
Gout, a type of arthritis that develops when needle-like crystals of uric acid deposit in the joints, most often those of the big toe
Juvenile idiopathic arthritis, the most common form of arthritis in children, which may be accompanied by fevers and rashes
Infectious arthritis, or arthritis that's caused by an infection, such as Lyme disease or Neisseria gonorrhoeae, the bacteria behind gonorrhea
Psoriatic arthritis, a type of arthritis (and also considered a spondyloarthropathy) that affects the fingers and toes and is associated with the skin disease psoriasis
Polymyositis, which affects the muscles and can affect the entire body
Bursitis, an inflammation of the bursas small fluid-filled sacs that reduce friction between bones
Ankylosing spondylitis, the most common spondyloarthropathy, which may affect the hips, shoulders, and knees, in addition to the spine
Reactive arthritis, or Reiter's syndrome, a spondyloarthropathy that develops after an infection of the urinary tract, bowels, or other organs
Scleroderma, or systemic sclerosis, an autoimmune rheumatic disease that leads to a thickening and tightening of the skin and inflammation and scarring in various other parts of the body, including the blood vessels, joints, and certain organs
Polymyalgia rheumatic, which causes pain and stiffness in tendons, muscles, ligaments, and tissues around joints
Rheumatic Disease Causes and Risk Factors
Experts believe rheumatic diseases are caused by a combination of genes and environmental factors. In general, having certain gene variants can increase a person's susceptibility to rheumatic diseases, and factors in the environment may trigger the onset of the disease.
For instance, studies suggest that people with certain variations of human leukocyte antigen (HLA) genes — which help control immune responses — have an increased risk of developing rheumatoid arthritis. In these people, the disease may develop due to some kind of triggering events, such as hormonal spikes, infections from bacteria or viruses, or obesity.
Similarly, an inherited cartilage weakness combined with excessive joint stress may play a role in the development of osteoarthritis.
Various factors can put you at greater risk of developing one or more rheumatic diseases. For example:
Osteoarthritis is more common in older adults than younger adults
Women are far more likely than men to develop rheumatoid arthritis, scleroderma, fibromyalgia, and lupus
Gout and spondyloarthropathies are more common in men
Lupus most often affects African-Americans and Hispanics
Obesity and smoking increases your risk for a number of rheumatic diseases
Dietary factors may increase or decrease your risk for certain rheumatic diseases — gout is associated with diets high in purines, which are found in various types of meat
Rheumatic Disease Symptoms
The hallmark of these rheumatic diseases is inflammation.
For arthritis, inflammation typically causes one or more symptoms in the joints, including:
Pain
Stiffness, especially in the morning
Swelling
Warmth and redness
Tenderness
Difficulty using the joint normally
Rheumatic diseases may produce a wide variety of other symptoms, such as:
Fatigue
Eye inflammation or infections
Rashes and sores
Pain in the neck, spine, or back
Difficulty taking a deep breath
Muscle pain
Psoriatic arthritis
Psoriatic arthritis is a type of arthritis that develops in some people with the skin condition psoriasis. It typically causes affected joints to become inflamed (swollen), stiff and painful.
Like psoriasis, psoriatic arthritis is a long-term condition that can get progressively worse. In severe cases, there's a risk of the joints becoming permanently damaged or deformed, which may require surgical treatment.
However, with an early diagnosis and appropriate treatment, it's possible to slow down the progression of the condition and minimise or prevent permanent damage to the joints.
Symptoms of psoriatic arthritis
The pain, swelling and stiffness associated with psoriatic arthritis can affect any joint in the body, but the condition often affects the hands, feet, knees, neck, spine and elbows.
The severity of the condition can vary considerably from person to person. Some people may have severe problems affecting many joints, whereas others may only notice mild symptoms in 1 or 2 joints.
There may be times when your symptoms improve (known as remission) and periods when they get worse (known as flare-ups or relapses).
Relapses can be very difficult to predict, but can often be managed with medication when they do occur.
When to seek medical advice
See your GP if you experience persistent pain, swelling or stiffness in your joints – even if you haven't been diagnosed with psoriasis.
If you've been diagnosed with psoriasis, you should have check-ups at least once a year to monitor your condition. Make sure you let your doctor know if you're experiencing any problems with your joints.
Causes of psoriatic arthritis
Between 1 and 2 in every 5 people with psoriasis develop psoriatic arthritis.
It usually develops within 10 years of psoriasis being diagnosed, although some people may experience problems with their joints before they notice any symptoms affecting their skin.
Like psoriasis, psoriatic arthritis is thought to occur as a result of the immune system mistakenly attacking healthy tissue.
However, it's not clear why some people with psoriasis develop psoriatic arthritis and others don't.
Diagnosing psoriatic arthritis
If your doctor thinks you may have arthritis, they should refer you to a rheumatologist (a specialist in joint conditions) for an assessment.
A rheumatologist will usually be able to diagnose psoriatic arthritis if you have psoriasis and problems with your joints.
They'll also try to rule out other types of arthritis, such as rheumatoid arthritis and osteoarthritis.
A number of tests may be carried out to help confirm a diagnosis, including:
blood tests to check for signs of inflammation in your body and the presence of certain antibodies found in other types of arthritis
X-rays or scans of your joints
Treating psoriatic arthritis
The main aims of treatment will be to relieve your symptoms, slow the progression of the condition and improve your quality of life.
Biological treatments
Biological treatments are a newer form of treatment for psoriatic arthritis. You may be offered one of these treatments if:
your psoriatic arthritis hasn't responded to at least two different types of DMARD
you're not able to be treated with at least two different types of DMARD
Biological drugs work by stopping particular chemicals in the blood from activating your immune system to attack the lining of your joints.