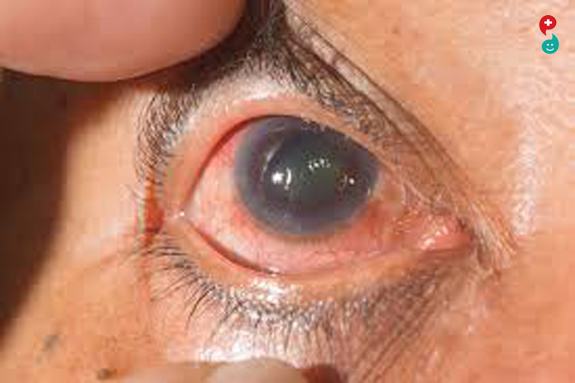
What Is Glaucoma?
Glaucoma is a condition that causes damage to your eye's optic nerve and gets worse over time. It's often linked to a buildup of pressure inside your eye. Glaucoma tends to be inherited and may not show up until later in life.
The increased pressure, called intraocular pressure, can damage the optic nerve, which transmits images to your brain. If the damage continues, glaucoma can lead to permanent vision loss. Without treatment, glaucoma can cause total permanent blindness within a few years.
Most people with glaucoma have no early symptoms or pain. You need to see your eye doctor regularly so she can diagnose and treat glaucoma before long-term visual loss happens.
If you’re over age 40 and have a family history of the disease, you should get a complete eye exam from an eye doctor every 1 to 2 years. If you have health problems like diabetes or a family history of glaucoma or are at risk for other eye diseases, you may need to go more often.
What Causes Glaucoma?
It’s the result of an intrinsic deterioration of the optic nerve, which leads to high fluid pressure on the front part of the eye.
Normally, the fluid, called aqueous humor, flows out of your eye through a mesh-like channel. If this channel gets blocked, the liquid builds up. The reason for the blockage is unknown, but doctors do know it can be inherited, meaning it’s passed from parents to children.
Less common causes include a blunt or chemical injury to your eye, severe eye infection, blocked blood vessels inside the eye, and inflammatory conditions. It’s rare, but sometimes eye surgery to correct another condition can bring it on. It usually affects both eyes, but it may be worse in one than the other.
What Are the Types of Glaucoma?
There are two main kinds:
Open-angle glaucoma. It’s the most common type. Your doctor may also call it wide-angle glaucoma. The drain structure in your eye -- it’s called the trabecular meshwork -- looks normal, but fluid doesn’t flow out like it should.
Angle-closure glaucoma. It’s less common in the West than in Asia. You may also hear it called acute or chronic angle-closure or narrow-angle glaucoma. Your eye doesn’t drain right because the drain space between your iris and cornea becomes too narrow. This can cause a sudden buildup of pressure in your eye. It’s also linked to farsightedness and cataracts, a clouding of the lens inside your eye.
Who Gets Glaucoma?
It mostly affects adults over 40, but young adults, children, and even infants can have it. African-Americans tend to get it more often, when they're younger, and with greater vision loss.
You’re more likely to get it if you:
Are of African-American, Irish, Russian, Japanese, Hispanic, Inuit, or Scandinavian descent
Are over 40
Have a family history of glaucoma
Have poor vision
Have diabetes
Take certain steroid medications, like prednisone
Have had trauma to the eye or eyes
What Are the Symptoms?
Most people don’t have any. The first sign is often a loss of peripheral, or side, vision. That can go unnoticed until late in the disease. That’s why glaucoma is often called the "sneak thief of vision."
Detecting glaucoma early is one reason you should have a complete exam with an eye specialist every 1 to 2 years. Occasionally, pressure inside the eye can rise to severe levels. In these cases, you may have sudden eye pain, headache, blurred vision, or the appearance of halos around lights.
If you have any of the following symptoms, seek immediate medical care:
Seeing halos around lights
Vision loss
Redness in the eye
Eye that looks hazy (particularly in infants)
Nausea or vomiting
Eye pain
Narrowed vision (tunnel vision)
How Is It Diagnosed?
Your eye doctor will use drops to open (he’ll call it dilate) your pupils. Then he’ll test your vision and examine your eyes. He’ll check your optic nerve, and if you have glaucoma, it will look a certain way. He may take photographs of the nerve to help him track your disease over time. He’ll do a test called tonometry to check your eye pressure. He’ll also do a visual field test, if necessary, to figure out if you've lost your side, or peripheral, vision. Glaucoma tests are painless and take very little time.
How Is Glaucoma Treated?
Your doctor may use prescription eye drops, laser surgery, or microsurgery to lower pressure in the eye.
Eye drops. These either reduce the formation of fluid in the eye or increase its outflow, thereby lowering eye pressure. Side effects may include allergies, redness, stinging, blurred vision, and irritated eyes. Some glaucoma drugs may affect your heart and lungs. Be sure to tell your doctor about any other medications you’re taking or are allergic to.
Laser surgery. This procedure can slightly increase the flow of the fluid from the eye for people with open-angle glaucoma. It can stop fluid blockage if you have angle-closure glaucoma. Procedures include:
Trabeculoplasty: Opens the drainage area
Iridotomy: Makes a tiny hole in the iris to let fluid flow more freely
Cyclophotocoagulation: Treats areas of the middle layer of your eye to reduce fluid production
Microsurgery. In a procedure called a trabeculectomy, the doctor creates a new channel to drain the fluid and ease eye pressure. Sometimes this form of glaucoma surgery fails and has to be redone. Your doctor might implant a tube to help drain fluid. Surgery can cause temporary or permanent vision loss, as well as bleeding or infection.
Open-angle glaucoma is most often treated with various combinations of eye drops, laser trabeculoplasty, and microsurgery. Doctors in the U.S. tend to start with medications, but there’s evidence that early laser surgery or microsurgery could work better for some people.
Infant or congenital glaucoma -- meaning you are born with it -- is primarily treated with surgery, because the cause of the problem is a very distorted drainage system.
Talk to your eye doctor to find out which glaucoma treatment is right for you.

Dry eyes
Overview
Dry eyes is a common condition that occurs when your tears aren't able to provide adequate lubrication for your eyes. Tears can be inadequate for many reasons. For example, dry eyes may occur if you don't produce enough tears or if you produce poor-quality tears.
Dry eyes feel uncomfortable. If you have dry eyes, your eyes may sting or burn. You may experience dry eyes in certain situations, such as on an airplane, in an air-conditioned room, while riding a bike or after looking at a computer screen for a few hours.
Treatments for dry eyes may make you more comfortable. These treatments can include lifestyle changes and eyedrops. You'll likely need to take these measures indefinitely to control the symptoms of dry eyes.
Symptoms
Signs and symptoms, which usually affect both eyes, may include:
A stinging, burning or scratchy sensation in your eyes
Stringy mucus in or around your eyes
Sensitivity to light
Eye redness
A sensation of having something in your eyes
Difficulty wearing contact lenses
Difficulty with nighttime driving
Watery eyes, which is the body's response to the irritation of dry eyes
Blurred vision or eye fatigue
When to see a doctor
See your doctor if you've had prolonged signs and symptoms of dry eyes, including red, irritated, tired or painful eyes. Your doctor can take steps to determine what's bothering your eyes or refer you to a specialist.
Causes
Dry eyes are caused by a lack of adequate tears. Your tears are a complex mixture of water, fatty oils and mucus. This mixture helps make the surface of your eyes smooth and clear, and it helps protect your eyes from infection.
For some people, the cause of dry eyes is decreased tear production. For others it's increased tear evaporation and an imbalance in the makeup of your tears.
Decreased tear production
Dry eyes can occur when you're unable to produce enough tears. The medical term for this condition is keratoconjunctivitis sicca (ker-uh-toe-kun-junk-tih-VY-tis SIK-uh). Common causes of decreased tear production include:
Aging
Certain medical conditions, including diabetes, rheumatoid arthritis, lupus, scleroderma, Sjogren's syndrome, thyroid disorders and vitamin A deficiency
Certain medications, including antihistamines, decongestants, hormone replacement therapy, antidepressants, and drugs for high blood pressure, acne, birth control and Parkinson's disease
Laser eye surgery, though symptoms of dry eyes related to this procedure are usually temporary
Tear gland damage from inflammation or radiation
Increased tear evaporation
Common causes of increased tear evaporation include:
Wind, smoke or dry air
Blinking less often, which tends to occur when you're concentrating, for example, while reading, driving or working at a computer
Eyelid problems, such as out-turning of the lids (ectropion) and in-turning of the lids (entropion)
Imbalance in tear composition
The tear film has three basic layers: oil, water and mucus. Problems with any of these layers can cause dry eyes. For example, the oil film produced by small glands on the edge of your eyelids (meibomian glands) might become clogged. Blocked meibomian glands are more common in people with inflammation along the edge of their eyelids (blepharitis), rosacea or other skin disorders.
Risk factors
Factors that make it more likely that you'll experience dry eyes include:
Being older than 50. Tear production tends to diminish as you get older. Dry eyes are more common in people over 50.
Being a woman. A lack of tears is more common in women, especially if they experience hormonal changes due to pregnancy, using birth control pills or menopause.
Eating a diet that is low in vitamin A, which is found in liver, carrots and broccoli, or low in omega-3 fatty acids, which are found in fish, walnuts and vegetable oils
Wearing contact lenses
Complications
People who have dry eyes may experience these complications:
Eye infections. Your tears protect the surface of your eyes from infection. Without adequate tears, you may have an increased risk of eye infection.
Damage to the surface of your eyes. If left untreated, severe dry eyes may lead to eye inflammation, abrasion of the corneal surface, corneal ulcer and vision problems.
Decreased quality of life. Dry eyes can make it difficult to perform everyday activities, such as reading.
Prevention
If you experience dry eyes, pay attention to the situations that are most likely to cause your symptoms. Then find ways to avoid those situations in order to prevent your dry eyes symptoms. For instance:
Avoid air blowing in your eyes. Don't direct hair dryers, car heaters, air conditioners or fans toward your eyes.
Add moisture to the air. In winter, a humidifier can add moisture to dry indoor air.
Consider wearing wraparound sunglasses or other protective eyewear. Safety shields can be added to the tops and sides of eyeglasses to block wind and dry air. Ask about shields where you buy your eyeglasses.
Take eye breaks during long tasks. If you're reading or doing another task that requires visual concentration, take periodic eye breaks. Close your eyes for a few minutes. Or blink repeatedly for a few seconds to help spread your tears evenly over your eyes.
Be aware of your environment. The air at high altitudes, in desert areas and in airplanes can be extremely dry. When spending time in such an environment, it may be helpful to frequently close your eyes for a few minutes at a time to minimize evaporation of your tears.
Position your computer screen below eye level. If your computer screen is above eye level, you'll open your eyes wider to view the screen. Position your computer screen below eye level so that you won't open your eyes as wide. This may help slow the evaporation of your tears between eye blinks.
Stop smoking and avoid smoke. If you smoke, ask your doctor for help devising a quit-smoking strategy that's most likely to work for you. If you don't smoke, stay away from people who do. Smoke can worsen dry eyes symptoms.
Use artificial tears regularly. If you have chronic dry eyes, use eyedrops even when your eyes feel fine to keep them well-lubricated.

Infertility
What is infertility?
Infertility is defined as not being able to get pregnant (conceive) after one year (or longer) of unprotected sex. Because fertility in women is known to decline steadily with age, some providers evaluate and treat women aged 35 years or older after 6 months of unprotected sex. Women with infertility should consider making an appointment with a reproductive endocrinologist—a doctor who specializes in managing infertility. Reproductive endocrinologists may also be able to help women with recurrent pregnancy loss, defined as having two or more spontaneous miscarriages.
Pregnancy is the result of a process that has many steps.
To get pregnant
A woman’s body must release an egg from one of her ovaries (ovulation).
A man’s sperm must join with the egg along the way (fertilize).
The fertilized egg must go through a fallopian tube toward the uterus (womb).
The fertilized egg must attach to the inside of the uterus (implantation).
Infertility may result from a problem with any or several of these steps.
Impaired fecundity is a condition related to infertility and refers to women who have difficulty getting pregnant or carrying a pregnancy to term.
Is infertility just a woman's problem?
No, infertility is not always a woman’s problem. Both men and women can contribute to infertility.
Many couples struggle with infertility and seek help to become pregnant, but it is often thought of as only a woman’s condition. However, in about 35% of couples with infertility, a male factor is identified along with a female factor. In about 8% of couples with infertility, a male factor is the only identifiable cause.
What causes infertility in men?
Infertility in men can be caused by different factors and is typically evaluated by a semen analysis. When a semen analysis is performed, the number of sperm (concentration), motility (movement), and morphology (shape) are assessed by a specialist. A slightly abnormal semen analysis does not mean that a man is necessarily infertile. Instead, a semen analysis helps determine if and how male factors are contributing to infertility.
Disruption of testicular or ejaculatory function
Varicoceles, a condition in which the veins on a man’s testicles are large and cause them to overheat. The heat may affect the number or shape of the sperm.
Trauma to the testes may affect sperm production and result in lower number of sperm.
Unhealthy habits such as heavy alcohol use, smoking, anabolic steroid use, and illicit drug use.
Use of certain medications and supplements.
Cancer treatment involving the use of certain types of chemotherapy, radiation, or surgery to remove one or both testicles
Medical conditions such as diabetes, cystic fibrosis, certain types of autoimmune disorders, and certain types of infections may cause testicular failure.
Hormonal disorders
Improper function of the hypothalamus or pituitary glands. The hypothalamus and pituitary glands in the brain produce hormones that maintain normal testicular function. Production of too much prolactin, a hormone made by the pituitary gland (often due to the presence of a benign pituitary gland tumor), or other conditions that damage or impair the function of the hypothalamus or the pituitary gland may result in low or no sperm production.
These conditions may include benign and malignant (cancerous) pituitary tumors, congenital adrenal hyperplasia, exposure to too much estrogen, exposure to too much testosterone, Cushing’s syndrome, and chronic use of medications called glucocorticoids.
Genetic disorders
Genetic conditions such as a Klinefelter’s syndrome, Y-chromosome microdeletion, myotonic dystrophy, and other, less common genetic disorders may cause no sperm to be produced, or low numbers of sperm to be produced.
What causes infertility in women?
Women need functioning ovaries, fallopian tubes, and a uterus to get pregnant. Conditions affecting any one of these organs can contribute to female infertility. Some of these conditions are listed below and can be evaluated using a number of different tests.
Disruption of ovarian function (presence or absence of ovulation (anovulation) and effects of ovarian “age”)
A woman’s menstrual cycle is, on average, 28 days long. Day 1 is defined as the first day of “full flow.” Regular predictable periods that occur every 24 to 32 days likely reflect ovulation. A woman with irregular periods is likely not ovulating.
Ovulation can be predicted by using an ovulation predictor kit and can be confirmed by a blood test to check the woman’s progesterone level on day 21 of her menstrual cycle. Although several tests exist to evaluate a woman’s ovarian function, no single test is a perfect predictor of fertility. The most commonly used markers of ovarian function include follicle-stimulating hormone (FSH) value on day 3 to 5 of the menstrual cycle, anti-müllerian hormone value (AMH), and antral follicle count (AFC) using a transvaginal ultrasound.
Disruptions in ovarian function may be caused by several conditions and warrants an evaluation by a doctor.
When a woman doesn’t ovulate during a menstrual cycle, it’s called anovulation. Potential causes of anovulation include the following
Polycystic ovary syndrome (PCOS). PCOS is a condition that causes women to not ovulate, or to ovulate irregularly. Some women with PCOS have elevated levels of testosterone, which can cause acne and excess hair growth. PCOS is the most common cause of female infertility.
Diminished ovarian reserve (DOR). Women are born with all of the eggs that they will ever have, and a woman’s egg count decreases over time. Diminished ovarian reserve is a condition in which there are fewer eggs remaining in the ovaries than normal. The number of eggs a woman has declines naturally as a woman ages. It may also occur due to congenital, medical, surgical, or unexplained causes. Women with a diminished ovarian reserve may be able to conceive naturally but will produce fewer eggs in response to fertility treatments.
Functional hypothalamic amenorrhea (FHA). FHA is a condition caused by excessive exercise, stress, or low body weight. It is sometimes associated with eating disorders such as anorexia.
Improper function of the hypothalamus and pituitary glands. The hypothalamus and pituitary glands in the brain produce hormones that maintain normal ovarian function. Production of too much of the hormone prolactin by the pituitary gland (often as the result of a benign pituitary gland tumor), or improper function of the hypothalamus or pituitary gland, may cause a woman not to ovulate.
Premature ovarian insufficiency (POI). POI, sometimes referred to as premature menopause, occurs when a woman’s ovaries fail before she is 40 years of age. Although certain exposures, such as chemotherapy or pelvic radiation therapy, and certain medical conditions may cause POI, the cause is often unexplained. About 5% to10% of women with POI conceive naturally and have a normal pregnancy.
Menopause Menopause is an age-appropriate decline in ovarian function that usually occurs around age 50. By definition, a woman in menopause has not had a period in one year. She may experience hot flashes, mood changes, difficulty sleeping, and other symptoms as well.
Fallopian tube obstruction (whether fallopian tubes are open, blocked, or swollen)
Risk factors for blocked fallopian tubes (tubal occlusion) can include a history of pelvic infection, history of ruptured appendicitis, history of gonorrhea or chlamydia, known endometriosis, or a history of abdominal surgery.
Tubal evaluation may be performed using an X-ray that is called a hysterosalpingogram (HSG), or by chromopertubation (CP) in the operating room at time of laparoscopy, a surgical procedure in which a small incision is made and a viewing tube called a laparoscope is inserted.
Hysterosalpingogram (HSG) is an X-ray of the uterus and fallopian tubes. A radiologist injects dye into the uterus through the cervix and simultaneously takes X-ray pictures to see if the dye moves freely through fallopian tubes. This helps evaluate tubal caliber (diameter) and patency.
Chromopertubation is similar to an HSG but is done in the operating room at the time of a laparoscopy. Blue-colored dye is passed through the cervix into the uterus and spillage and tubal caliber (shape) is evaluated.
Abnormal uterine contour (physical characteristics of the uterus)
Depending on a woman’s symptoms, the uterus may be evaluated by transvaginal ultrasound to look for fibroids or other anatomic abnormalities. If suspicion exists that the fibroids may be entering the endometrial cavity, a sonohystogram (SHG) or hysteroscopy (HSC) may be performed to further evaluate the uterine environment.
How long should couples try to get pregnant before seeing a doctor?
Most experts suggest at least one year for women younger than age 35. However, for women aged 35 years or older, couples should see a health care provider after 6 months of trying unsuccessfully. A woman’s chances of having a baby decrease rapidly every year after the age of 30.
Some health problems also increase the risk of infertility. So, couples with the following signs or symptoms should not delay seeing their health care provider when they are trying to become pregnant
Irregular periods or no menstrual periods.
Very painful periods.
Endometriosis.
Pelvic inflammatory disease.
More than one miscarriage.
Suspected male factor (i.e., history of testicular trauma, hernia surgery, chemotherapy, or infertility with another partner).
It is a good idea for any woman and her partner to talk to a health care provider before trying to get pregnant. They can help you get your body ready for a healthy baby, and can also answer questions on fertility and give tips on conceiving.
How will doctors find out if a woman and her partner have fertility problems?
Doctors will begin by collecting a medical and sexual history from both partners. The initial evaluation usually includes a semen analysis, a tubal evaluation, and ovarian reserve testing.
How do doctors treat infertility?
Infertility can be treated with medicine, surgery, intrauterine insemination, or assisted reproductive technology.
Often, medication and intrauterine insemination are used at the same time. Doctors recommend specific treatments for infertility on the basis of
The factors contributing to infertility.
The duration of infertility.
The age of the female.
The couple’s treatment preference after counseling about success rates, risks, and benefits of each treatment option.
What are some of the specific treatments for male infertility?
Male infertility may be treated with medical, surgical, or assisted reproductive therapies depending on the underlying cause. Medical and surgical therapies are usually managed by an urologist who specializes in infertility. A reproductive endocrinologist may offer intrauterine inseminations (IUIs) or in vitro fertilization (IVF) to help overcome male factor infertility.
What medicines are used to treat infertility in women?
Some common medicines used to treat infertility in women include
Clomiphene citrate is a medicine that causes ovulation by acting on the pituitary gland. It is often used in women who have polycystic ovary syndrome (PCOS) or other problems with ovulation. It is also used in women with normal ovulation to increase the number of mature eggs produced. This medicine is taken by mouth.
Letrozole is a medication that is frequently used off-label to cause ovulation. It works by temporarily lowering a woman’s progesterone level, which causes the brain to naturally make more FSH. It is often used to induce ovulation in a woman with PCOS, and in women with normal ovulation to increase the number of mature eggs produced in the ovaries.
What is a hernia?
A hernia occurs when an internal organ or other body part protrudes through the wall of muscle or tissue that normally contains it. Most hernias occur within the abdominal cavity, between the chest and the hips.
The most common forms of hernia are:
Inguinal hernia: In men, the inguinal canal is a passageway for the spermatic cord and blood vessels leading to the testicles. In women, the inguinal canal contains the round ligament that gives support for the womb. In an inguinal hernia, fatty tissue or a part of the intestine pokes into the groin at the top of the inner thigh. This is the most common type of hernia, and affects men more often than women.
Femoral hernia: Fatty tissue or part of the intestine protrudes into the groin at the top of the inner thigh. Femoral hernias are much less common than inguinal hernias and mainly affect older women.
Umbilical hernia: Fatty tissue or part of the intestine pushes through the abdomen near the navel (belly button).
Hiatal (hiatus) hernia: Part of the stomach pushes up into the chest cavity through an opening in the diaphragm (the horizontal sheet of muscle that separates the chest from the abdomen).
Other types of hernias include:
Incisional hernia: Tissue protrudes through the site of an abdominal scar from a remote abdominal or pelvic operation.
Epigastric hernia: Fatty tissue protrudes through the abdominal area between the navel and lower part of the sternum (breastbone).
Spigelian hernia: The intestine pushes through the abdomen at the side of the abdominal muscle, below the navel.
Diaphragmatic hernia: Organs in the abdomen move into the chest through an opening in the diaphragm.
What is the incidence of hernias?
Of all hernias that occur:
75–80% are inguinal or femoral
2% are incisional or ventral
3–10% are umbilical, affecting 10-20% of newborns; most close by themselves by 5 years of age
1–3% are other types
What causes a hernia?
Inguinal and femoral hernias are due to weakened muscles that may have been present since birth, or are associated with aging and repeated strains on the abdominal and groin areas. Such strain may come from physical exertion, obesity, pregnancy, frequent coughing, or straining on the toilet due to constipation.
Adults may get an umbilical hernia by straining the abdominal area, being overweight, having a long-lasting heavy cough or after giving birth.
The cause of hiatal hernias is not fully understood, but a weakening of the diaphragm with age or pressure on the abdomen could play a part.
What are the symptoms of a hernia?
A hernia in the abdomen or groin can produce a noticeable lump or bulge that can be pushed back in, or that can disappear when lying down. Laughing, crying, coughing, straining during a bowel movement, or physical activity may make the lump reappear after it has been pushed in. More symptoms of a hernia include:
Swelling or bulge in the groin or scrotum (the pouch that contains the testicles)
Increased pain at the site of the bulge
Pain while lifting
Increase in the bulge size over time
A dull aching sensation
A sense of feeling full or signs of bowel obstruction
In the case of hiatal hernias there are no bulges on the outside of the body. Instead, symptoms may include heartburn, indigestion, difficulty swallowing, frequent regurgitation (bringing food back up) and chest pain.
A heart attack happens when there is a sudden complete blockage of an artery that supplies blood to an area of your heart.
A heart is a muscle, and it needs a good blood supply to keep it healthy.
As we get older, the smooth inner walls of the arteries that supply the blood to the heart can become damaged and narrow due to the build up of fatty materials, called plaque.
When an area of plaque breaks, blood cells and other parts of the blood stick to the damaged area and form blood clots. A heart attack occurs when a blood clot completely blocks the flow of blood and seriously reduces blood flow to the heart muscle. This also results in patients experiencing chest pain.
As a result, some of the heart muscle starts to die.
The longer the blockage is left untreated, the more the heart muscle is damaged. If the blood flow is not restored quickly, the damage to the heart muscle is permanent.
A heart attack is sometimes called a myocardial infarction (MI), acute myocardial infarction, coronary occlusion or coronary thrombosis.
A heart attack happens when there is a sudden complete blockage of an artery that supplies blood to an area of your heart.
1
2
3
4
Causes
The underlying cause of a heart attack is coronary heart disease.
Some people may not know they have coronary heart disease until they have a heart attack. For others, a heart attack can happen after weeks, months or years of having coronary heart disease.
Symptoms
Heart attack warning signs can vary from person to person, and they may not always be sudden or severe. Read about heart attack warning signs
Diagnosis
If you are rushed to hospital with a suspected heart attack, your health care team will do some tests to find out if you are having a heart attack. They may include:
electrocardiogram (ECG)
blood tests
chest X-ray
coronary angiogram.
These tests will help them to decide the best treatment for you. Find out more about medical tests
Treatment
Emergency treatment
If you think you’re having a heart attack, call Triple Zero (000). Don’t hang up. Ask the operator for an ambulance. Too many people lose their lives because they wait too long to get treatment for heart attack.
You may be given medicines to help dissolve clots.
There is a high risk of dangerous changes to your heartbeat after the start of a heart attack. The most serious changes stop your heart beating and cause a cardiac arrest. Ambulance or hospital staff may use a defibrillator to give your heart a controlled electric shock that may make it start beating again.
In hospital
In hospital, you will receive treatments that help to reduce damage to your heart, and to help prevent future problems. You may need to have a procedure like:
angioplasty and stent implantation
bypass surgery (also known as coronary artery bypass grafts or CABG).
Read more about heart procedures and devices
Preventing further problems
Medical treatments and healthy lifestyle choices can help your heart attack recovery, greatly reduce your risk of further heart problems, and relieve or control symptoms such as angina. Read about living with heart disease
Cardiac rehabilitation
If you’ve had a heart attack or a procedure, you should be given information about a cardiac rehabilitation program which is another really important step in your recovery.