Overview
Myasthenia gravis (my-us-THEE-nee-uh GRAY-vis) is characterized by weakness and rapid fatigue of any of the muscles under your voluntary control.
Myasthenia gravis is caused by a breakdown in the normal communication between nerves and muscles.
There is no cure for myasthenia gravis, but treatment can help relieve signs and symptoms, such as weakness of arm or leg muscles, double vision, drooping eyelids, and difficulties with speech, chewing, swallowing and breathing.
Though myasthenia gravis can affect people of any age, it's more common in women younger than 40 and in men older than 60.
Myasthenia gravis care at Mayo Clinic
Symptoms
Muscle weakness caused by myasthenia gravis worsens as the affected muscle is used repeatedly. Because symptoms usually improve with rest, your muscle weakness may come and go. However, myasthenia gravis symptoms tend to progress over time, usually reaching their worst within a few years after the onset of the disease.
Although myasthenia gravis can affect any of the muscles that you control voluntarily, certain muscle groups are more commonly affected than others.
Eye muscles
In more than half the people who develop myasthenia gravis, their first signs and symptoms involve eye problems, such as:
Drooping of one or both eyelids (ptosis).
Double vision (diplopia), which may be horizontal or vertical, and improves or resolves when one eye is closed.
Face and throat muscles
In about 15 percent of people with myasthenia gravis, the first symptoms involve face and throat muscles, which can cause:
Altered speaking. Your speech may sound very soft or nasal, depending upon which muscles have been affected.
Difficulty swallowing. You may choke very easily, which makes it difficult to eat, drink or take pills. In some cases, liquids you're trying to swallow may come out your nose.
Problems chewing. The muscles used for chewing may wear out halfway through a meal, particularly if you've been eating something hard to chew, such as steak.
Limited facial expressions. Your family members may comment that you've "lost your smile" if the muscles that control your facial expressions have been affected.
Neck and limb muscles
Myasthenia gravis can cause weakness in your neck, arms and legs, but this usually happens along with muscle weakness in other parts of your body, such as your eyes, face or throat.
The disorder usually affects arms more often than legs. However, if it affects your legs, you may waddle when you walk. If your neck is weak, it may be hard to hold up your head.
When to see a doctor
Talk to your doctor if you have difficulty:
Breathing
Seeing
Swallowing
Chewing
Walking
Using your arms or hands
Holding up your head
Causes
Antibodies
Your nerves communicate with your muscles by releasing chemicals (neurotransmitters) that fit precisely into receptor sites on the muscle cells at the nerve-muscular junction.
In myasthenia gravis, your immune system produces antibodies that block or destroy many of your muscles' receptor sites for a neurotransmitter called acetylcholine (as-uh-teel-KOH-leen). With fewer receptor sites available, your muscles receive fewer nerve signals, resulting in weakness.
Antibodies may also block the function of a protein called a muscle-specific receptor tyrosine kinase (TIE-roh-seen KIE-nays). This protein is involved in forming the nerve-muscular junction. When antibodies block the function of this protein, it may lead to myasthenia gravis. Research continues to study how the antibodies inhibiting this protein are related to the development of myasthenia gravis.
Thymus gland
Researchers believe that the thymus gland, a part of your immune system situated in the upper chest beneath your breastbone, may trigger or maintain the production of the antibodies that block acetylcholine.
Large in infancy, the thymus is small in healthy adults. In some adults with myasthenia gravis, however, the thymus is abnormally large. Some people with myasthenia gravis also have tumors of the thymus (thymomas). Usually, thymomas aren't cancerous (malignant).
Other causes
Some people may have myasthenia gravis that isn't caused by antibodies blocking acetylcholine or the muscle-specific receptor tyrosine kinase. This type of myasthenia gravis is called antibody-negative myasthenia gravis. Antibodies against another protein, called lipoprotein-related protein 4, may play a part in the development of this condition.
Genetic factors also may be associated with myasthenia gravis.
Rarely, mothers with myasthenia gravis have children who are born with myasthenia gravis (neonatal myasthenia gravis). If treated promptly, children generally recover within two months after birth.
Some children are born with a rare, hereditary form of myasthenia, called congenital myasthenic syndrome.
Factors that can worsen myasthenia gravis
Fatigue
Illness
Stress
Some medications — such as beta blockers, quinidine gluconate, quinidine sulfate, quinine (Qualaquin), phenytoin (Dilantin), certain anesthetics and some antibiotics
Complications
Complications of myasthenia gravis are treatable, but some can be life-threatening.
Myasthenic crisis
Myasthenic crisis is a life-threatening condition that occurs when the muscles that control breathing become too weak to do their jobs. Emergency treatment is needed to provide mechanical assistance with breathing. Medications and blood-filtering therapies help people to again breathe on their own.
Thymus tumors
About 15 percent of people with myasthenia gravis have a tumor in their thymus, a gland under the breastbone that is involved with the immune system. Most of these tumors, called thymomas, aren't cancerous (malignant).
Other disorders
People with myasthenia gravis are more likely to have the following conditions:
Underactive or overactive thyroid. The thyroid gland, which is in the neck, secretes hormones that regulate your metabolism. If your thyroid is underactive, you may have difficulties dealing with cold, weight gain and other issues. An overactive thyroid can cause difficulties dealing with heat, weight loss and other issues.
Autoimmune conditions. People with myasthenia gravis may be more likely to have autoimmune conditions, such as rheumatoid arthritis or lupus.
The symptoms of facial palsy are many and vary from person to person. The symptoms will depend on the cause of your facial palsy and here we discuss some of the more common symptoms experienced.
How quickly do symptoms occur?
The onset of your symptoms may be sudden (appearing overnight), or may appear over two or three days. Alternatively, your symptoms may develop slowly over time (over weeks, or even months). In either situation, you should visit your GP as soon as possible, as further investigations may be required. It is important that you have a clear diagnosis of the cause so that you are given the correct treatment and advice.
What are the symptoms of facial palsy?
Facial palsy normally affects only one side of the face although in rare cases it may affect both sides. It does not cause weakness in your arms or legs. If you experience weakness in your arms or legs as well as weakness on one side of your face, you should seek immediate medical attention. These symptoms grouped together may indicate a stroke.
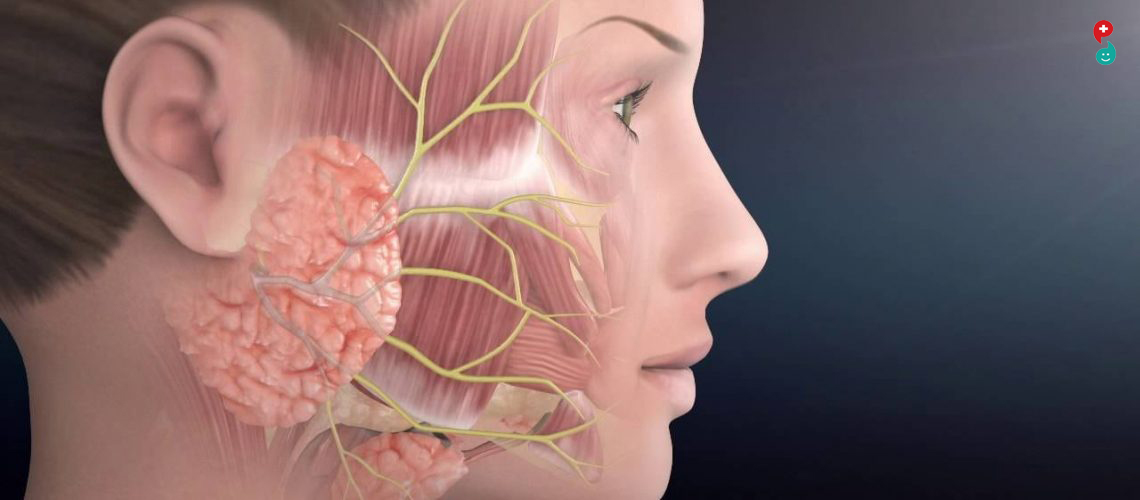
A complete facial palsy on one side of the face affects the brow, eye, cheek, and mouth. This means the facial nerve signals that control movement in these muscles are not working. The face may appear flattened and movement may be lost.
Symptoms may improve or worsen over time depending on the type and degree of facial nerve damage and the cause of your facial palsy.
Some types of facial palsy will affect sensation including pain, as well as facial movement. This may mean that the nerve which is responsible for sensation (trigeminal nerve) has been damaged as well as the facial nerve. The facial nerve controls movement, tear production, saliva production and taste.
Loss of sensation may mean you cannot feel your face when you touch it.
Inability to blink or close the eye is a common symptom and needs prompt attention from your GP.
How does facial palsy affect facial muscles and facial function?
Forehead
Loss of forehead wrinkles and inability to frown
Eye area
Droopy eyebrow and inability to raise an eyebrow
Inability to close the eye fully or blink
Watery eye or dry eye
Inability to squint
Drooping of the lower eyelid which may make the eye appear wide
Painful eye with symptoms of grittiness or irritation
Sensitivity to light
Soreness or redness of the white of the eye
Please note: seek prompt advice from your GP if you are experiencing any problems with your eyes.
Mouth
The corner of the mouth pulls down/droops
Inability to smile on the affected side
Inability to puff up your cheeks, whistle or blow
Altered taste
Tingling of the affected half of the tongue
Difficulty eating and drinking
Difficulty brushing your teeth and spitting out
Drooling from the weak corner of your mouth
Excess or reduced salivation (dry mouth)
Inability to pout
Difficulty speaking because of weakness in the lips and cheek
Ear(s)
Pain in or near the affected ear
Loss of hearing
Increased sensitivity to high pitched noise
Nose
Nose runs or feels stuffy
Inability to flare nostril
Inability to wrinkle nose
If a person develops symptoms of facial palsy slowly (over weeks or months) then they should immediately be referred for further investigations.
Bell's palsy causes sudden, temporary weakness in your facial muscles. This makes half of your face appear to droop. Your smile is one-sided, and your eye on that side resists closing.
Bell's palsy, also known as facial palsy, can occur at any age. The exact cause is unknown. It's believed to be the result of swelling and inflammation of the nerve that controls the muscles on one side of your face. Or it might be a reaction that occurs after a viral infection.
For most people, Bell's palsy is temporary. Symptoms usually start to improve within a few weeks, with complete recovery in about six months. A small number of people continue to have some Bell's palsy symptoms for life. Rarely, Bell's palsy can recur.
Symptoms
Facial weakness
Facial paralysis
Signs and symptoms of Bell's palsy come on suddenly and may include:
Rapid onset of mild weakness to total paralysis on one side of your face — occurring within hours to days
Facial droop and difficulty making facial expressions, such as closing your eye or smiling
Drooling
Pain around the jaw or in or behind your ear on the affected side
Increased sensitivity to sound on the affected side
Headache
A decrease in your ability to taste
Changes in the amount of tears and saliva you produce
In rare cases, Bell's palsy can affect the nerves on both sides of your face
Causes
Although the exact reason Bell's palsy occurs isn't clear, it's often related to exposure to a viral infection. Viruses that have been linked to Bell's palsy include the virus that causes:
Cold sores and genital herpes (herpes simplex)
Chickenpox and shingles (herpes zoster)
Infectious mononucleosis (Epstein-Barr)
Cytomegalovirus infections
Respiratory illnesses (adenovirus)
German measles (rubella)
Mumps (mumps virus)
Flu (influenza B)
Hand-foot-and-mouth disease (coxsackievirus)
The nerve that controls your facial muscles passes through a narrow corridor of bone on its way to your face. In Bell's palsy, that nerve becomes inflamed and swollen — usually related to a viral infection. Besides facial muscles, the nerve affects tears, saliva, taste and a small bone in the middle of your ear.
Risk factors
Bell's palsy occurs more often in people who:
Are pregnant, especially during the third trimester, or who are in the first week after giving birth
Have an upper respiratory infection, such as the flu or a cold
Have diabetes
Recurrent attacks of Bell's palsy are rare. But in some of these cases, there's a family history of recurrent attacks — suggesting a possible genetic predisposition to Bell's palsy.