Catecholamine blood test
This test measures the levels of catecholamines in the blood. Catecholamines are hormones made by the adrenal glands. The three catecholamines are epinephrine (adrenalin), norepinephrine, and dopamine.
Catecholamines are more often measured with a urine test than with a blood test.
How the Test is Performed
A blood sample is needed.
How to Prepare for the Test
You will likely be told not to eat anything (fast) for 10 hours before the test. You may be allowed to drink water during this time.
The accuracy of the test can be affected by certain foods and medicines. Foods that can increase catecholamine levels include:
Coffee
Tea
Bananas
Chocolate
Cocoa
Citrus fruits
Vanilla
You should not eat these foods for several days before the test. This is especially true if both blood and urine catecholamines are to be measured.
You should also avoid stressful situations and vigorous exercise. Both can affect the accuracy of the test results.
Medicines and substances that can increase catecholamine measurements include:
Acetaminophen
Albuterol
Aminophylline
Amphetamines
Buspirone
Caffeine
Calcium channel blockers
Cocaine
Cyclobenzaprine
Levodopa
Methyldopa
Nicotinic acid (large doses)
Phenoxybenzamine
Phenothiazines
Pseudoephedrine
Reserpine
Tricyclic antidepressants
Medicines that can decrease catecholamine measurements include:
Clonidine
Guanethidine
MAO inhibitors
If you take any of the above medicines, check with your health care provider before the blood test about whether you should stop taking your medicine.
How the Test will Feel
When the needle is inserted to draw blood,some people feel slight pain. Others feel a prick or stinging. Afterward, there may be some throbbing or a slight bruise. This soon goes away.
Why the Test is Performed
Catecholamines are released into the blood when a person is under physical or emotional stress. The main catecholamines are dopamine, norepinephrine, and epinephrine (which used to be called adrenalin).
This test is used to diagnose or rule out certain rare tumors,such as pheochromocytoma or neuroblastoma. It may also be done in patients with those conditions to determine if treatment is working.
Normal Results
The normal range for epinephrine is 0 to 140 pg/mL (764.3 pmol/L).
The normal range for norepinephrine is 70 to 1700 pg/mL (413.8 to 10048.7 pmol/L).
The normal range for dopamine is 0 to 30 pg/mL (195.8 pmol/L).
Note: Normal value ranges may vary slightly among different laboratories. Some labs use different measurements or test different samples. Talk to your provider about the meaning of your specific test results.
What Abnormal Results Mean
Higher-than-normal levels of blood catecholamines may suggest:
Acute anxiety
Ganglioblastoma (very rare tumor)
Ganglioneuroma (very rare tumor)
Neuroblastoma (rare tumor)
Pheochromocytoma (rare tumor)
Severe stress
Additional conditions under which the test may be performed include multiple system atrophy.
Risks
Veins and arteries vary in size from one person to another,and from one side of the body to the other. Taking blood from some people may be more difficult than from others.
Other risks associated with having blood drawn are slight, but may include:
Excessive bleeding
Fainting or feeling lightheaded
Hematoma (blood accumulating under the skin)
Infection (a slight risk any time the skin is broken)
Alternative Names
Norepinephrine - blood; Epinephrine - blood; Adrenalin - blood; Dopamine - blood.
Carbohydrate antigen 19-9 (CA19-9) test
CA19-9 is the common term for carbohydrate antigen sialyl Lewis a. It is a protein found on the surface of certain cancer cells. It may be found in the blood when it is shed by cancer cells.
CA19-9 is commonly used as a tumour marker for some types of cancer of the pancreas.But this test cannot be used by itself to find pancreatic or other cancers because:
CA19-9 is also found in healthy adults in small amounts in the pancreas, liver,gallbladder and lungs.
About 5% of people do not produce CA19-9,so this test cannot be used for them.
The blood levels of this antigen may also be at a higher than normal level in healthy people and in people with non-cancerous conditions such as pancreatitis or bile duct obstruction.
Why a CA19-9 test is done
A CA19-9 test is mainly used to:
check a person’s response to treatment for some types of pancreatic cancer, especially advanced pancreatic cancer
see if pancreatic cancer is still growing or has come back (recurred) after treatment
How a ca19-9 test is done
CA19-9 is usually measured by a blood test. The blood sample is sent to a lab to be tested.
What the results mean
A higher than normal level of CA19-9 can be found in healthy people and can also be found in people with non-cancerous and cancerous conditions.
Non-cancerous conditions include:
liver diseases, such as cirrhosis or hepatitis
inflammation of the gallbladder (cholecystitis) or gallstones
inflammation of the pancreas (pancreatitis)
cystic fibrosis
some disorders of the lung, kidney or gastrointestinal tract
Types of cancer include:
some types of pancreatic cancer
colorectal
stomach
liver
bile duct
lung
breast
uterine
ovarian
The highest levels of this antigen are most commonly seen in people with advanced pancreatic cancer. CA19-9 is not usually high in people with very early stages of the disease.
If CA19-9 levels have been higher than normal, a decrease in CA19-9 or a return to normal values may mean that the cancer is responding well to treatment. An increase may mean that the cancer is not responding well to treatment, is still growing or is coming back. A slight increase may not be important. The doctor compares the levels over time.
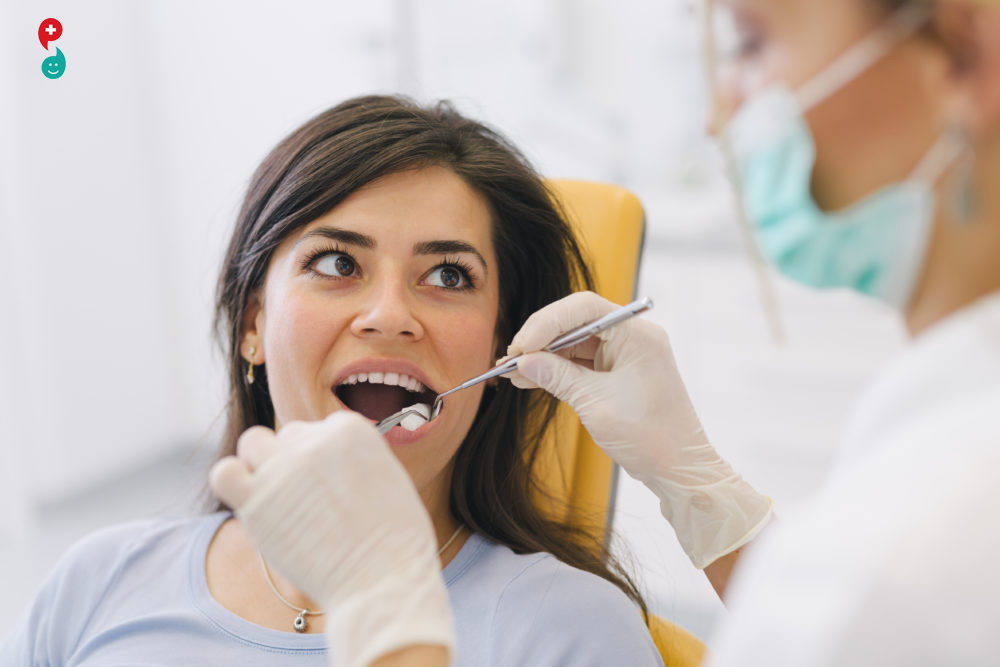
Wisdom tooth extraction
What is Wisdom tooth extraction?
Wisdom tooth extraction is a surgical procedure to remove one or more wisdom teeth — the four permanent adult teeth located at the back corners of your mouth on the top and bottom.
If a wisdom tooth doesn't have room to grow (impacted wisdom tooth), resulting in pain, infection or other dental problems, you'll likely need to have it pulled. Wisdom tooth extraction may be done by a dentist or an oral surgeon.
To prevent potential future problems, some dentists and oral surgeons recommend wisdom tooth extraction even if impacted teeth aren't currently causing problems.
Why it's done?
Wisdom teeth, or third molars, are the last permanent teeth to appear (erupt) in the mouth. These teeth usually appear between the ages of 17 and 25. Some people never develop wisdom teeth. For others, wisdom teeth erupt normally — just as their other molars did — and cause no problems.
Many people develop impacted wisdom teeth — teeth that don't have enough room to erupt into the mouth or develop normally. Impacted wisdom teeth may erupt only partially or not at all.
An impacted wisdom tooth may:
Grow at an angle toward the next tooth (second molar)
Grow at an angle toward the back of the mouth
Grow at a right angle to the other teeth, as if the wisdom tooth is "lying down" within the jawbone
Grow straight up or down like other teeth but stay trapped within the jawbone
Problems with impacted wisdom teeth
You'll likely need your impacted wisdom tooth pulled if it results in problems such as:
Pain
Trapping food and debris behind the wisdom tooth
Infection or gum disease (periodontal disease)
Tooth decay in a partially erupted wisdom tooth
Damage to a nearby tooth or surrounding bone
Development of a fluid-filled sac (cyst) around the wisdom tooth
Complications with orthodontic treatments to straighten other teeth
Preventing future dental problems
Dental specialists disagree about the value of extracting impacted wisdom teeth that aren't causing problems (asymptomatic).
It's difficult to predict future problems with impacted wisdom teeth. However, here's the rationale for preventive extraction:
Symptom-free wisdom teeth could still harbor disease.
If there isn't enough space for the tooth to erupt, it's often hard to get to it and clean it properly.
Serious complications with wisdom teeth happen less often in younger adults.
Older adults may experience difficulty with surgery and complications after surgery.
Risks:
Most wisdom tooth extractions don't result in long-term complications. However, removal of impacted wisdom teeth occasionally requires a surgical approach that involves making an incision in the gum tissue and removing bone. Rarely, complications can include:
Painful dry socket, or exposure of bone when the post-surgical blood clot is lost from the site of the surgical wound (socket)
Infection in the socket from bacteria or trapped food particles
Damage to nearby teeth, nerves, jawbone or sinuses
How you prepare?
Your dentist may perform the procedure in the office. However, if your tooth is deeply impacted or if the extraction requires an in-depth surgical approach, your dentist may suggest you see an oral surgeon. In addition to making the area numb with local anesthetic, your surgeon may suggest sedation to allow you to be more comfortable during the procedure.
Questions to ask:
Questions you may want to ask your dentist or oral surgeon include:
How many wisdom teeth need to be removed?
What type of anesthesia will I receive?
How complicated do you expect the procedure to be?
How long is the procedure likely to last?
Have the impacted wisdom teeth caused damage to other teeth?
Is there a risk that I might have nerve damage?
What other dental treatments might I need at a later date?
How long does it take to completely heal and return to normal activity?
Preparing for surgery:
A wisdom tooth extraction is almost always performed as an outpatient procedure. This means that you go home the same day.
You'll receive instructions from the hospital or dental clinic staff on what to do before the surgery and the day of your scheduled surgery.
When to call your dentist or surgeon?
Call your dentist or oral surgeon if you experience any of the following signs or symptoms, which could indicate an infection, nerve damage or other serious complication:
Difficulty swallowing or breathing
Excessive bleeding
Fever
Severe pain not relieved by prescribed pain medications
Swelling that worsens after two or three days
A bad taste in your mouth not removed with saltwater rinsing
Pus in or oozing from the socket
Persistent numbness or loss of feeling
Blood or pus in nasal discharge
Results:
You probably won't need a follow-up appointment after a wisdom tooth extraction if:
You don't need stitches removed
No complications arose during the procedure
You don't experience persistent problems, such as pain, swelling, numbness or bleeding — complications that might indicate infection, nerve damage or other problems
If complications develop, contact your dentist or oral surgeon to discuss treatment options.
WHISPER TEST
What is whisper test?
A hearing test provides an evaluation of the sensitivity of a person's sense of hearing and is most often performed by an audiologist using an audiometer. An audiometer is used to determine a person's hearing sensitivity at different frequencies. There are other hearing tests as well, e.g., Weber test and Rinne test.
Ear examination:
Prior to the hearing test itself, the ears of the client are usually examined with an otoscope to make sure they are free of wax, that the eardrum is intact, the ears are not infected, and the middle ear is free of fluid (indicating middle ear infection). The most common reasons to develop hearing loss due to genetic disorder, ageing problems, exposure to noise pollution, infections, birth complications, trauma to the ear, and certain medications or toxins.
Pure tone audiometry
The standard and most common type of hearing test is pure tone audiometry, which measures the air and bone conduction thresholds for each ear in a set of 8 standard frequencies from 250Hz to 8000Hz. The test is conducted in a sound booth using either a pair of foam inserts or supraural headphones connected to an external audiometer. The result of the test is an audiogram diagram which plots a person's hearing sensitivity at the tested frequencies. On an audiogram an "x" plot represents the softest threshold heard at each specific frequency in the left ear, and an "o" plot represents the softest threshold heard at each specific frequency in the right ear. There is also a high frequency version of the test which tests frequencies over 8000Hz to 16000Hz which may be employed in special circumstances.
Instructions
The examiner stands at arm's length (~0.6 m) behind the patient (to prevent lip reading)
The opposite auditory canal is occluded by the patient or examiner and the tragus is rubbed in a circular motion (goal; to block hearing from that ear)
The examiner exhales and whispers a combination of numbers and letters (example 4-K-2). Whispering at the end of exhalation is to ensure as quiet and as standardized voice as possible.
If the patient responds correctly, hearing is considered normal and no further screening is necessary on that ear.
If the patient responds incorrectly, then repeat using a different number-letter combination.
If on repeated testing, the patient can answer three out of a possible six numbers-letters correctly, the patient passes. If they cannot answer three out of six or more, the patient fails in that ear.
Repeat the sequence in the opposite ear using different combinations of numbers and letters. (Note: patients with memory problems may need a simplified letter/number combination to compensate for their inability to remember)
Significance
Hearing loss prohibits patients from understanding conversations, contributes to cognitive decline, and leads to social isolation. This impairment is the third most chronic impairment among older people. It is also useful to ask the patient and family if they
have noticed any changes in hearing, to describe any changes and if they have had any prior treatment.
Patients with no wax occlusion of their ear canal and who failed this test have a hearing loss that correlates with 30 dB loss. This level of hearing loss has a significant affect on communication.
You've probably already been told how important it is to conduct a self-examination of your breasts regularly, in order to ensure that no abnormal lumps or bumps have formed. What's less well known is that a vulvar self-exam – an at-home exam to check for possible abnormalities concerning your vulva – can also be worthwhile.
Why Should Women Perform a Vulvar Self-Exam?
Not to be confused with the vagina, the vulva is the external genitals, made up of the labia majora, the labia minora, and the clitoris. By performing a vulvar self-exam, you'll be able to spot any abnormalities that may indicate infection, vulvar cancer, or other conditions before they become a larger problem.
A vulvar self-exam can also be useful in teaching you what is normal in appearance for your vulva. No two vulvas look alike, and becoming familiar with the appearance of your vulva will ensure that, if abnormalities do develop in the future, you'll notice.
How Often Should a Woman Do a Vulvar Self-Exam?
This exam should be done about once a month, in between menstrual cycles. If you are no longer menstruating, you should set a regular date on which to perform a vulvar self-exam.
Do I Require Any Special Equipment in Order to Conduct This Exam?
You need only two things to perform a vulvar self-examination: a private area to perform the exam, where you won't be interrupted, and a mirror. The exam itself should only take about five to 10 minutes.
How Do I Perform a Vulvar Self-Exam?
1. Stand, squat, or sit over the top of a handheld mirror, making sure you can see your genitals clearly. If it makes things easier, you may ask your partner to assist you with this.
2. Check the area where your pubic hair grows. Look for any moles, spots, lesions, bumps, or rashes.
3. Next, find your clitoris. Look for any growths, bumps, or discoloration.
4. Check your labia majora (the outer lips) and feel for any bumps. Also, visually look for any moles, rashes, growths, or lesions.
5. Repeat this check with your labia minora (the inner lips).
6. Finally, look at your perineum. The perineum is the space located between the vagina and the anus. Again, look for rashes, bumps, growths, and lesions.
Report anything suspicious or abnormal to your doctor, even if it seems to be small.
Further Reading
Vulvar cancer is a rare type of cancer that affects the vulva. There are several types of vulvar cancer and, in the early stages, it rarely has any symptoms. As the disease progresses, however, symptoms can include moles, lumps, or bumps on the vulva, which is why performing a regular self-examination is so important.
One of the main reasons for the high cure rate of skin cancer is the ability to detect it in its early stages. However, early detection relies on people taking an active role in their healthcare by learning how to check their bodies for potentially cancerous spots.