What is tuberculosis?
Tuberculosis is an infectious disease that usually affects the lungs. Compared with other diseases caused by a single infectious agent, tuberculosis is the second biggest killer globally. TB usually affects the lungs, although it can spread to other organs around the body. Doctors make a distinction between two kinds of tuberculosis infection: latent and active.
Latent TB: The bacteria remain in the body in an inactive state. They cause no symptoms and are not contagious, but they can become active.
Active TB: The bacteria do cause symptoms and can be transmitted to others.
About one-third of the world's population is believed to have latent TB. There is a 10 percent chance of latent TB becoming active, but this risk is much higher in people who have compromised immune systems, i.e., people living with HIV or malnutrition, or people who smoke. TB affects all age groups and all parts of the world. However, the disease mostly affects young adults and people living in developing countries.
What are the warning signs?
Feeling sick or weak
Loss of appetite and weight loss
Chills, fever, and night sweats
A severe cough that lasts for 3 weeks or more
Chest pain
TB can also affect other parts of the body. Symptoms will depend on the part it affects.
What are the symptoms?
During a latent stage, TB has no symptoms. When TB is active TB, while TB usually affects the lungs, it can also affect other parts of the body, and the symptoms will vary accordingly. Without treatment, TB can spread to other parts of the body through the bloodstream.
Bones: There may be spinal pain and joint destruction.
Brain: It can lead to meningitis.
Liver and kidneys: It can impair the waste filtration functions and lead to blood in the urine.
Heart: It can impair the heart's ability to pump blood, resulting in cardiac tamponade, a condition that can be fatal.
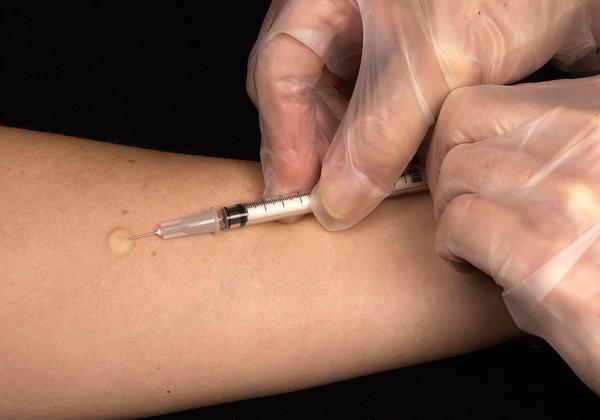
What are the available diagnoses?
The most common diagnostic test for TB is a skin test where a small injection of PPD tuberculin, an extract of the TB bacterium, is made just below the inside forearm. The injection site should be checked after 2-3 days, and, if a hard, red bump has swollen up to a specific size, then it is likely that TB is present. Unfortunately, the skin test is not 100 percent accurate and has been known to give incorrect positive and negative readings. There are other tests that are available to diagnose TB. Blood tests, chest X-rays, and sputum tests can all be used to test for the presence of TB bacteria and may be used alongside a skin test.
What are the treatments?
The precise type and length of antibiotic treatment depend on a person's age, overall health, potential resistance to drugs, whether the TB is latent or active, and the location of infection (i.e., the lungs, brain, kidneys). People with latent TB may need just one kind of TB antibiotics, whereas people with active TB (particularly MDR-TB) will often require a prescription of multiple drugs.
Antibiotics are usually required to be taken for a relatively long time. The standard length of time for a course of TB antibiotics is about 6 months. TB medication can be toxic to the liver, and although side effects are uncommon, when they do occur, they can be quite serious. Potential side effects should be reported to a doctor and include:
Dark urine
Fever
Jaundice
Loss of appetite
Nausea and vomiting
It is important for any course of treatment to be completed fully, even if the TB symptoms have gone away. Any bacteria that have survived the treatment could become resistant to the medication that has been prescribed and could lead to developing MDR-TB in the future.
What are the causes?
The Mycobacterium tuberculosis bacterium causes TB. It is spread through the air when a person with TB (whose lungs are affected) coughs, sneezes, spits, laughs, or talks. TB is contagious, but it is not easy to catch. The chances of catching TB from someone you live or work with are much higher than from a stranger. Most people with active TB who have received appropriate treatment for at least 2 weeks are no longer contagious. Since antibiotics began to be used to fight TB, some strains have become resistant to drugs. Multidrug-resistant TB (MDR-TB) arises when an antibiotic fails to kill all of the bacteria, with the surviving bacteria developing resistance to that antibiotic and often others at the same time.
What are the preventions?
Face mask
If you have active TB, a face mask can help lower the risk of the disease spreading to other people
A few general measures can be taken to prevent the spread of active TB
Avoiding other people by not sleeping in the same room as someone, will help to minimize the risk of germs from reaching anyone else
Wearing a mask, covering the mouth, and ventilating rooms can also limit the spread of bacteria
Drug-Resistant TB
What is Drug-Resistant TB?
Tuberculosis (TB) is a disease caused by bacteria that are spread from person to person through the air. TB usually affects the lungs, but it can also affect other parts of the body, such as the brain, the kidneys, or the spine. In most cases,TB is treatable and curable; however, people with TB can die if they do not get proper treatment. Sometimes drug-resistant TB occurs when bacteria become resistant to the drugs used to treat TB.This means that the drug can no longer kill the TB bacteria.
Drug-resistant TB (DR TB)is spread the same way that drug-susceptible TB is spread.TB is spread through the air from one person to another.The TB bacteria are put into the air when a person with TB disease of the lungs or throat coughs,sneezes, speaks, or sings. People nearby may breathe in these bacteria and become infected.
Causes of Drug Resistant TB
Drug-resistant TB can occur when the drugs used to treat TB are misused or mismanaged. Examples of misuse or mismanagement include
People do not complete a full course of TB treatment
Health care providers prescribe the wrong treatment (the wrong dose or length of time)
Drugs for proper treatment are not available
Drugs are of poor quality
Drug-resistant TB is more common in people who
Do not take their TB drugs regularly
Do not take all of their TB drugs
Develop TB disease again, after being treated for TB disease in the past
Come from areas of the world where drug-resistant TB is common
Have spent time with someone known to have drug-resistant TB disease
Types of Drug Resistant TB
Multidrug-Resistant TB (MDR TB)
Multidrug-resistant TB (MDR TB) is caused by TB bacteria that is resistant to at least isoniazid and rifampin, the two most potent TB drugs. These drugs are used to treat all persons with TB disease.
TB experts should be consulted in the treatment of MDR TB.
Extensively Drug-resistant TB (XDR TB)
Extensively drug-resistant TB (XDR TB) is a rare type of MDR TB that is resistant to isoniazid and rifampin, plus any fluoroquinolone and at least one of three injectable second-line drugs (i.e., amikacin, kanamycin, or capreomycin).
Because XDR TB is resistant to the most potent TB drugs, patients are left with treatment options that are much less effective.
XDR TB is of special concern for people with HIV infection or other conditions that can weaken the immune system. These people are more likely to develop TB disease once they are infected, and also have a higher risk of death once they develop TB.
TB experts should be consulted in the treatment of XDR TB.
Laboratory Guidance
The emergence of Mycobacterium tuberculosis strains that cause XDR TB has prompted the issuance of interim guidelines for clinical and research laboratories handling XDR TB specimens
Prevention of Drug-Resistant TB
The most important way to prevent the spread of drug-resistant TB is to take all TB drugs exactly as prescribed by the health care provider. No doses should be missed and treatment should not be stopped early. People receiving treatment for TB disease should tell their health care provider if they are having trouble taking the drugs.
Health care providers can help prevent drug-resistant TB by quickly diagnosing cases, following recommended treatment guidelines, monitoring patients’ response to treatment, and making sure therapy is completed.
Another way to prevent getting drug-resistant TB is to avoid exposure to known drug-resistant TB patients in closed or crowded places such as hospitals, prisons, or homeless shelters. People who work in hospitals or health-care settings where TB patients are likely to be seen should consult infection control or occupational health experts.
Treatment of Drug-Resistant TB
Drug-resistant TB is caused by TB bacteria that are resistant to at least one first-line anti-TB drug. Multidrug-resistant TB (MDR TB) is resistant to more than one anti-TB drug and at least isoniazid (INH) and rifampin (RIF).
Extensively drug-resistant TB (XDR TB) is a rare type of MDR TB that is resistant to isoniazid and rifampin, plus any fluoroquinolone and at least one of three injectable second-line drugs (i.e., amikacin, kanamycin, or capreomycin).
Treating and curing drug-resistant TB is complicated. Inappropriate management can have life-threatening results. Drug-resistant TB should be managed by or in close consultation with an expert in the disease.
patients receiving fluoroquinolone antibacterial drugs for tuberculosis (TB) also have a chance of experiencing the adverse effects noted by FDA, fluoroquinolone antibacterial drugs are absolutely necessary for some patients who have drug-resistant TB disease or drug-resistant latent TB infection or who cannot tolerate first-line TB drugs. For these TB patients, there are no better alternatives, and the benefits of fluoroquinolone antibacterial drugs outweigh the risks because TB is not a minor infection, but potentially fatal or debilitating.
A cough is probably one of the most common respiratory diseases that people suffer from. In most cases, it is nothing to worry about and can be cured with cough suppressants and salt water gargles. However, coughing of blood is a serious problem. The coughing up of blood that originates from below the level of the larynx is known as hemoptysis. This can vary in terms of severity depending on the amount of blood being expelled. This disease is a common condition, but on an average, less than 5% of hemoptysis cases are life threatening.
Hemoptysis rarely affects children. The symptoms of this condition include:
Sudden onset of a cough with bloody phlegm
1.Fever
2.Anorexia and weight loss
3.Dyspnoea
4.Paroxysmal nocturnal dyspnoea
5.Fatigue
Chest pain: Medical attention should be sought in cases where this condition recurs often, if it lasts for longer than a fortnight or if the volume of blood expectorated is more than 30ml per day. The various tools that help in the diagnosis of this condition are:
Chest radiography: This imaging modality helps lateralize bleeding and understand the amount of lung involvement. It is quick, inexpensive and can also help detect other underlying abnormalities.
Bronchoscopy: This involves the insertions of a rigid or flexible endoscope into the bronchial passages to check the airways and determine active bleeding sites.
MDCT: A multidetector CT is a non-invasive imaging tool that provides a comprehensive evaluation of airways, lung parenchyma, and thoracic vessels. It can also be used to uncover potential causes of bleeding such as bronchiectasis, pulmonary infections and lung cancer. In some cases, a multidetector CT angiography may also be used.
Oral antibiotics are usually the first stage of treatment for this condition. Smokers will also be urged to quit cigarettes as this can worsen their condition. Treatment for minor hemoptysis may also include:
1.Oral hemostatics
2.Cough suppressants
3.Anticoagulants
4.Radiation of laser treatment
5.Therapeutic bronchoscopy
In its later stages, hemoptysis can be treated with a minimally invasive procedure known as endovascular embolization or with surgery. In some cases, endovascular embolization may also be sued to stabilise the patient before surgery. This procedure reduces the pressure in the hypertrophic arterial blood vessels and decreases the risk of perioperative bleeding.
Hemoptysis is also one of the most common complaints of lung cancer patients. Depending on the stage of cancer and the amount of blood expectorated, treatment in some cases may not be possible. In such cases, a parenteral opioid and fast-acting benzodiazepine may be administered.
Tuberculosis can be cured with anti-TB medication. As treatment for TB takes much longer than other types of bacterial infections, a patient is often required to take a combination of drugs for six to nine months.
Even if the symptoms of tuberculosis begin to disappear after you’ve begun taking the drugs, it is imperative to continue taking them for the entire course to ensure that all TB germs are killed, says Dr Low Su Ying, Senior Consultant, Department of Respiratory & Critical Care Medicine, Singapore General Hospital (SGH), a member of the SingHealth group.
“Incomplete TB treatment will allow the surviving TB germs to continue to grow and multiply. But this time, they may develop resistance to the first-line drugs. In such situations, second-line TB drugs must be taken for a longer period but the chance of cure is considerably reduced,” explains Dr Low.
Prevention tips for tuberculosis (TB)
Here are the measures you can adopt to help protect yourself and others from tuberculosis:
-Go for a check-up if you suspect that you could be suffering from TB.
-Keep your immune system functioning properly by adopting healthy eating habits, exercising regularly and getting sufficient sleep.
-If someone you know has contracted TB, encourage him or her to adhere faithfully to the treatment.
If you have been diagnosed with active TB, be sure to:
-Complete the full course of your TB medications.
-Stay at home especially during the first two weeks of treatment.
-Cover your mouth with a tissue when you cough or -sneeze, and wear a face mask when around people during the first few weeks of treatment.
क्षय रोगाचे निदान (टीबी) निदान करण्यासाठी, आपला आरोग्य सेवा प्रदाता संपूर्ण इतिहासाच्या दरम्यान आणि शारीरिक तपासणी दरम्यान माहितीचे पाच महत्वाचे भाग गोळा करेल:
लक्षणे
एक्सपोजरचा इतिहास
टीबीसाठी ट्यूबरक्युलिन त्वचा चाचणी किंवा रक्त तपासणी
चेस्ट एक्स-रे किंवा छाती सीटी स्कॅन
स्पुटम टेस्ट
टीबीसाठी आपली चाचणी घ्यावी जर:
आपल्याला वाटत असेल की आपल्याकडे सक्रिय टीबी रोग आहे.
आपण ज्या व्यक्तीस ओळखत आहात किंवा संशयित टीबी रोग आहे अशा व्यक्तीशी आपण वेळ घालवला आहे.
आपण एचआयव्ही संसर्गग्रस्त आहात किंवा दुसर्या प्रकारची स्थिती आहे जी आपल्याला सक्रिय टीबी रोगास जास्त धोका देते.
आपण अशा देशाचे आहात जेथे सक्रिय टीबी रोग बराच सामान्य आहे (लॅटिन अमेरिका, कॅरिबियन, आफ्रिका आणि आशिया व पूर्वी यूरोप व रशियामधील बहुतेक देश).
जेथे आपण टीबी रोग अधिक सामान्य असतो अशा ठिकाणी राहणे किंवा कार्य करणे, जसे बेघर निवारा, स्थलांतरित फार्म कॅम्प, जेल किंवा तुरुंग, किंवा काही नर्सिंग होम.
आपण बेकायदेशीर इंट्राव्हेनस औषधे वापरता.
एक्सपोजरचा इतिहास
टीबीचे निदान आणि उपचार करण्यात अचूक इतिहास घेणे महत्वाचे आहे. कोणत्याही आजाराप्रमाणे, लवकर हस्तक्षेप आणि उपचार खूप महत्वाचे आहे.
ट्यूबरक्युलिन स्किन टेस्ट
ट्यूबरक्युलिन त्वचा चाचणी (किंवा पीपीडी) ने घातलेल्या टीबी रोगाचे एक अर्क वापरते. मारल्या गेलेल्या त्वचेचा त्वचेत इंजेक्शन केला जातो. जर एखाद्या व्यक्तीस क्षयरोगाने संसर्ग झाला असेल तर इंजेक्शनच्या ठिकाणी एक गठ्ठा तयार केला जाईल. हे एक सकारात्मक चाचणी आहे. याचा अर्थ असा होतो की टीबीच्या रोगामुळे शरीराला संसर्ग झाला आहे. याचा अर्थ असा नाही की व्यक्तीस सक्रिय रोग आहे. सकारात्मक त्वचा असलेले लोक परीक्षण करतात परंतु सक्रिय रोगाशिवाय इतरांना संक्रमण प्रसारित करू शकत नाही.
टीबी साठी मागील लसीकरण ट्यूबरक्युलिन त्वचा चाचणीची वैधता तडजोड करते. नवीन रक्त तपासणीने खर्या टीबी संसर्ग झालेल्या लोकांना ओळखण्यात मदत केली आहे. अधिक जाणून घ्या.
क्षय रोग तपासणी
दोन नवीन रक्त तपासणी करण्यात आल्या आहेत ज्या अलीकडे तपेदिकांच्या रोगाशी निगडीत होण्यासाठी तपासण्यासाठी विकसित करण्यात आले आहेत. ते अजूनही संशोधन सेटिंग्जमध्ये वापरले जातात, परंतु काही रुग्णालये आणि क्लिनिक ते ट्यूबरकुलिन त्वचा चाचणीच्या जागी वापरत आहेत. प्रत्येक चाचण्यामध्ये रक्त संग्रहित करणे आवश्यक असते जे नंतर टीबी बनविणार्या बॅक्टेरियामध्ये आढळणार्या अँटीजन (प्रथिने) च्या गटासह उत्तेजित केले जाते. आपल्या प्रतिरक्षा प्रणालीने हे प्रतिजैव कधी पाहिले असेल, तर आपले पेशी इंटरफेरॉन-गामा तयार करतील, जी आपल्या प्रतिरक्षा प्रणालीद्वारे उत्पादित केलेले पदार्थ आणि प्रयोगशाळेत मोजले जाऊ शकतात. क्वांटिफेरॉन-टीबी® गोल्ड (क्यूएफटी) चाचणी आणि टी-स्पॉट® टीबी चाचणी दोन उपलब्ध आहेत. हे परीक्षण ट्यूबरकुलिन त्वचा चाचणीपेक्षा अधिक संवेदनशील आणि विशिष्ट असल्याचे दिसते. महत्वाचे म्हणजे, ट्यूबरक्युलिन त्वचा चाचण्यांप्रमाणे ते मागील बीसीजी लसीकरणामुळे प्रभावित होत नाहीत.
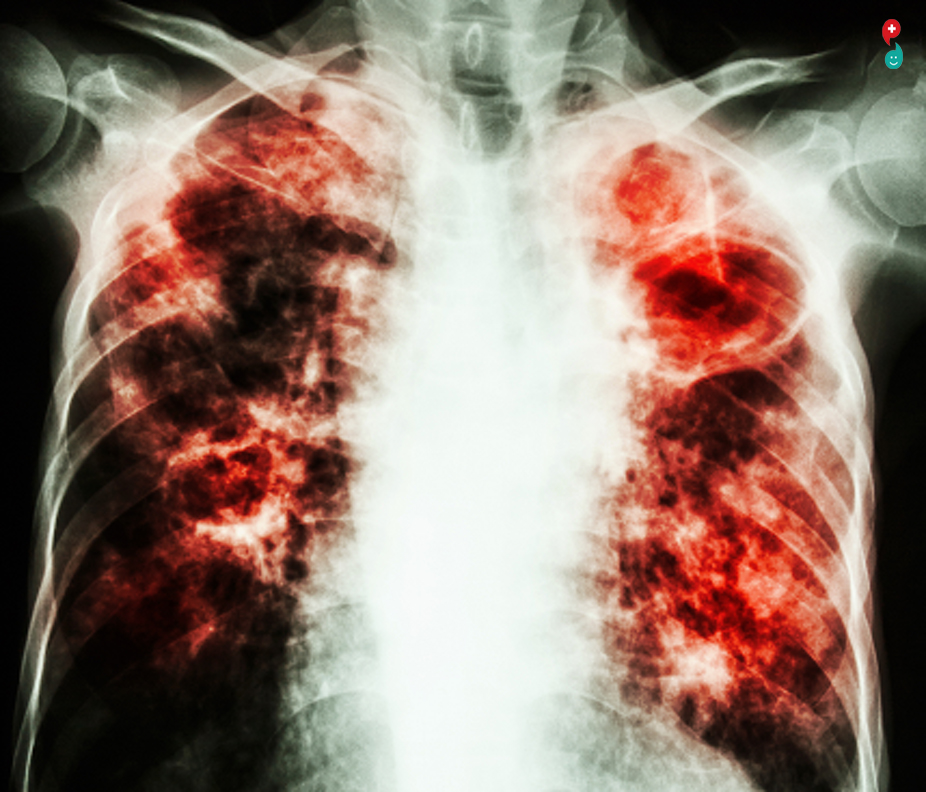
चेस्ट एक्स-रे
जर एखाद्या व्यक्तीस क्षयरोगाने संसर्ग झाला असेल परंतु सक्रिय रोग विकसित झाला नाही तर छातीचा एक्स-रे नेहमीच सामान्य असेल. सकारात्मक पीपीडी (त्वचा चाचणी) किंवा टीबी रक्त तपासणीसह बहुतेक लोक सामान्य छातीचे एक्स-किरण असतात आणि निरोगी राहतात. अशा लोकांसाठी, प्रतिबंधक औषधांची शिफारस केली जाऊ शकते.
तथापि, जर जीवाणूंनी फुफ्फुसावर हल्ला केला आणि जळजळ केला तर, छातीच्या एक्स-किरणांवर असामान्य सावली दिसू शकते. या लोकांसाठी, निदान चाचणी (स्वाद तपासणी) आणि उपचार सहसा योग्य आहेत. अधिक जाणून घ्या.
स्पुटम टेस्ट
फुफ्फुसांपासून बनवलेल्या फुलांचे नमुने तपासले जाऊ शकतात जे टीबी रोगास उपस्थित आहेत का हे पाहण्यासाठी. क्षयरोगांचे पुरावे पहाण्यासाठी सूक्ष्मदर्शिकेच्या ("स्टुमम स्मर") अंड्यातून बाहेर पडणे तपासले जाते. अधिक जाणून घ्या.