MBBS Obstetrics and Gynecologist Gynaecological Endoscopy Specialist 8 Years Experience, Maharashtra
Eating a variety of nutritious, colourful fruits and vegetables daily is key to preventing and lowering your risk of developing breast and other women’s cancers fuelled by obesity.
“Women should minimise the processed foods they eat from a box,”
“Natural, whole and fresh foods are always the best choices.”
One in eight women will develop breast cancer in their lifetime, but the good news is, if caught early, it can be treated effectively. Starting at age 40, go for an annual mammogram to check breast health and in between mammograms, perform monthly breast self-exams.
Colon cancer is the third largest cause of cancer death among women. “At age 50, women need to make sure they start getting their regular colonoscopy screening,” As catching any abnormal colon polyp growths early can prevent cancer from further developing or spreading.
“Cancers caused by smoking are preventable if you put the cigarettes down,”
More than 13% of women are still smoking cigarettes in the US, despite the evidence that it leads to premature death, heart disease, heart attack and stroke, and lung and other cancers.
#healthyeating #Nutrition #healthydiet
Overview
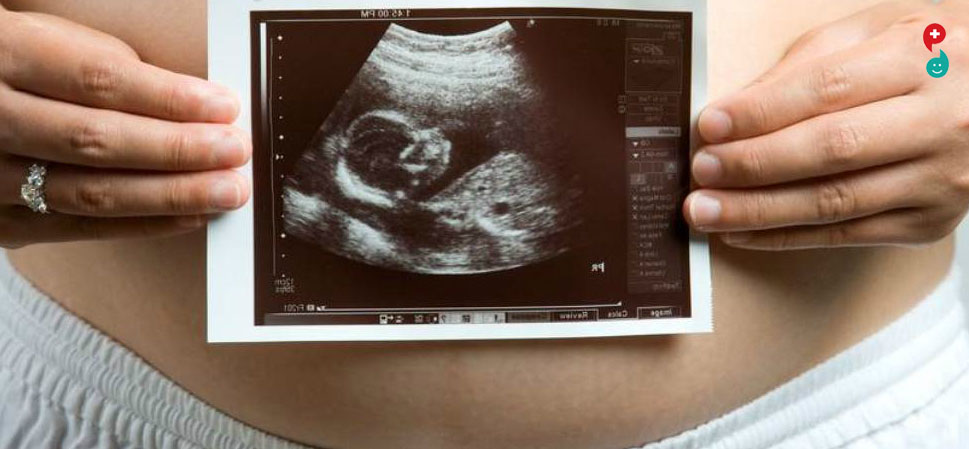
A fetal ultrasound (sonogram) is an imaging technique that uses sound waves to produce images of a fetus in the uterus. Fetal ultrasound images can help your health care provider evaluate your baby's growth and development and monitor your pregnancy. In some cases, fetal ultrasound is used to evaluate possible problems or help confirm a diagnosis.
The first fetal ultrasound is usually done during the first trimester to confirm the pregnancy and estimate how long you've been pregnant. If your pregnancy remains uncomplicated, the next ultrasound is typically offered during the second trimester, when anatomic details are visible. If a problem is suspected, a follow-up ultrasound or additional imaging tests, such as an MRI, might be recommended.
There are two main types of fetal ultrasound exams:
Transvaginal ultrasound. With this type of fetal ultrasound, a wandlike device called a transducer is placed in your vagina to send out sound waves and gather the reflections. Transvaginal ultrasounds are used most often during early pregnancy. This type of ultrasound also might be done if a transabdominal ultrasound didn't provide enough information.
Transabdominal ultrasound. A transabdominal fetal ultrasound is done by moving a transducer over your abdomen.
Various other types of transabdominal ultrasounds are available, including:
Specialized sonographic evaluation. This type of exam might be needed in specific circumstances, such as when a fetal abnormality is known or suspected. In this situation, a more detailed evaluation can provide additional information about the abnormality.
3D ultrasound. This exam provides a two-dimensional display of three-dimensional data. This type of ultrasound is sometimes used to help health care providers detect facial abnormalities or neural tube defects.
Doppler ultrasound. A Doppler ultrasound measures slight changes in the ultrasound waves as they bounce off moving objects, such as blood cells. It can provide details about a baby's blood flow.
Fetal echocardiography. This exam provides a detailed picture of a baby's heart. It might be used to confirm or rule out a congenital heart defect.
Why it's done
First trimester ultrasound examination is done to evaluate the presence, size and location of the pregnancy, determine the number of fetuses, and estimate how long you've been pregnant (gestational age). Ultrasound can also be used for first trimester genetic screening, as well as screening for abnormalities of your uterus or cervix.
In the second or third trimester a standard ultrasound is done to evaluate several features of the pregnancy, including fetal anatomy. This exam is typically done between weeks 18 and 20 of pregnancy. However, the timing of this ultrasound might be altered for reasons such as obesity, which could limit visualization of the fetus.
During the second and third trimesters, limited ultrasound evaluation might be needed when a specific question requires investigation. Examples include the evaluation of fetal growth and the estimation of amniotic fluid volume. A specialized or detailed exam is done when an anomaly is suspected based on your history or other prenatal exam results.
Your health care provider might use fetal ultrasound to:
Confirm the pregnancy and its location. Some fetuses develop outside of the uterus, in the fallopian tube. A fetal ultrasound can help your health care provider detect a pregnancy outside of the uterus (ectopic pregnancy).
Determine your baby's gestational age. Knowing the baby's age can help your health care provider determine your due date and track various milestones throughout your pregnancy.
Confirm the number of babies. If your health care provider suspects a multiple pregnancy, an ultrasound might be done to confirm the number of babies.
Evaluate your baby's growth. Your health care provider can use ultrasound to determine whether your baby is growing at a normal rate. Ultrasound can be used to monitor your baby's movement, breathing and heart rate.
Study the placenta and amniotic fluid levels. The placenta provides your baby with vital nutrients and oxygen-rich blood. Too much or too little amniotic fluid the fluid that surrounds the baby in the uterus during pregnancy or complications with the placenta need special attention. An ultrasound can help evaluate the placenta and amniotic fluid around the baby.
Identify birth defects. An ultrasound can help your health care provider screen for some birth defects.
Investigate complications. If you're bleeding or having other complications, an ultrasound might help your health care provider determine the cause.
Perform other prenatal tests. Your health care provider might use ultrasound to guide needle placement during certain prenatal tests, such as amniocentesis or chorionic villus sampling.
Determine fetal position before delivery. Most babies are positioned headfirst by the end of the third trimester. That doesn't always happen, though. Ultrasound imaging can confirm the baby's presentation so that your health care provider can discuss options for delivery.
Fetal ultrasound should be done only for valid medical reasons. Fetal ultrasound isn't recommended only to determine a baby's sex. Similarly, fetal ultrasound isn't recommended solely for the purpose of producing keepsake videos or pictures.
If your health care provider doesn't suggest a fetal ultrasound but you'd like the reassurance an ultrasound can provide, share your wishes with your care provider so that you can work together to determine what's best for you and your baby.
Risks
Diagnostic ultrasound has been used during pregnancy for many years and is generally considered safe when used appropriately. The lowest amount of ultrasound energy that provides an accurate assessment should be used.
Fetal ultrasound also has limitations. Fetal ultrasound might not detect all birth defects or might incorrectly suggest a birth defect is present when it's not.
How you prepare
You might be asked to drink a certain amount of fluid or avoid urinating before a fetal ultrasound, depending on the type of ultrasound. When scheduling your ultrasound, ask your health care provider for instructions.
Also be aware that fetal ultrasound can be done through the vagina (transvaginal) or over the abdomen (transabdominal), depending on why it's being done or the stage of your pregnancy. If you're having a transabdominal ultrasound, consider wearing loosefitting clothing so that you can easily expose your abdomen.
What you can expect
During the procedure
During a transabdominal fetal ultrasound, you'll recline on an exam table and expose your abdomen. Your health care provider or technician will apply a special gel to your abdomen. This will improve the conduction of sound waves and eliminate air between your skin and the transducer.
Your health care provider or technician will move or scan the transducer back and forth over your abdomen. The sound waves reflected off your bones and other tissues will be converted into images on a monitor.
Your health care provider or technician will measure your baby's anatomy. He or she might print or store certain images to document important structures. You'll likely be given copies of some of the images.
Depending on your baby's position and stage of development, you might be able to make out a face, hands and fingers, or arms and legs. Don't worry if you can't "see" your baby. Ultrasound images can be hard for an untrained observer to decipher. Ask your health care provider or technician to explain what's on the screen.
The procedure for other types of fetal ultrasound exams is similar. If you're having a transvaginal ultrasound, however, you'll be asked to change into a hospital gown or undress from the waist down. You'll recline on an exam table and place your feet in stirrups. The transducer will be covered in a plastic sheath, like a condom, and be lubricated with gel. Your health care provider or technician will place the transducer in your vagina.
After the procedure
You can wipe off any residual gel or lubricant. If you had a full bladder during the ultrasound, you can urinate after the exam.
Results
Typically, a fetal ultrasound offers reassurance that a baby is growing and developing normally. If your health care provider wants more details about your baby's health, he or she might recommend additional tests.
Pregnancy tests
You can often tell if you’re pregnant by noticing at least one common symptom. If you’re experiencing any of the symptoms of pregnancy, you should take a home pregnancy test or visit your doctor to confirm the pregnancy.
You’ll likely get accurate results from a pregnancy test one day after your first missed period. However, it’s best to wait at least a week after your missed period to be sure that you get the most accurate test results.
Home pregnancy tests
A home pregnancy test (HPT) can be used on the first day of your missed period. Some very sensitive tests can be used even earlier.
These tests work by detecting the hormone human chorionic gonadotropin (hCG) in your urine. This hormone is only found in the body during pregnancy. A chemical in the stick changes color when it comes into contact with this hormone. Waiting times will vary depending on the test, but most take about 10 minutes to deliver an accurate reading.
Most manufacturers recommend that HPTs be taken twice, since results may vary if you take a test too soon after your first missed period. In some cases, your hCG levels are too low to catch early on. Applicators vary from brand to brand, but the tests are generally inexpensive.
Pregnancy tests are accurate when they’re used correctly. It's possible to have a false negative, which happens when you’re pregnant but the test says you aren't. If you missed your period and it doesn’t arrive after a few days, repeat the test or check with your doctor.
Shop for home pregnancy tests.
Clinical urine test
You can get a clinical urine test at your doctor’s office. These tests aren’t necessarily more accurate than an HPT. However, your doctor may be able to help eliminate any possible errors that might affect the accuracy of the test. Depending on your health insurance plan, a clinical urine test may cost more than an HPT.
Results of a clinical urine test can vary depending on the medical facility that you visit. However, you can usually expect your results within a week of taking the test.
Blood test
These tests are taken at your doctor’s office. A laboratory tests your blood to detect hCG.
There are two types of pregnancy blood tests:
Qualitative hCG blood test: This test checks to see whether any hCG is being produced in the body. It gives a simple yes or no answer as to whether you’re pregnant.
Quantitative hCG blood test: This test measures the specific level of hCG in the blood.
If your hCG level is higher or lower than expected based on how far along you think you are in the pregnancy, your doctor may order further tests. They can include an ultrasound or repeat the hCG test in a couple of days. The most common reason for the hCG level to appear abnormal is being unsure about your dates. This would mean you are either further along in the pregnancy or not as far as you thought.
Quantitative hCG blood tests are very accurate because they measure the exact amount of hCG in the blood. They can detect smaller amounts of the hormone than a qualitative hCG blood test or a urine test.
Blood tests can detect hCG earlier than urine tests. Blood tests are usually more expensive than home tests, and you have to wait longer for your results. Blood test results can take more than a week, and sometimes two, to be delivered.
Early symptoms of pregnancy
Some symptoms of pregnancy are especially noticeable early on, including:
a missed period
feeling exhausted
urinating more than normal
sensitive, swollen breasts
nausea
vomiting
If you notice any of these symptoms, talk to your doctor, especially if you’ve recently had unprotected sex.

MD - Allopathy Gynaecological Endoscopy Specialist Infertility Specialist 12 Years Experience, Pune
Truth be told, no one knows why pregnancy cravings happen. Some experts say they may be nature's way of providing nutrients an expectant mom may be lacking. Others say they're an emotional thing. Regardless, as long as you're eating an overall healthy diet, it's usually OK to give in to your cravings. Just be careful to limit portions—don't down all that ice cream at once!—and know which snacks to steer clear of. A few foods to avoid: raw and undercooked meat or eggs; brie, feta, and other types of unpasteurized cheese; herbal teas; and raw sprouts.
Make Friends
Find ways to meet other pregnant women, whether that's through a prenatal yoga or childbirth class, a neighbourhood parents group, or an online parenting forum. The support, resources, and camaraderie from other women in the same boat as you can be crucial for getting through the ups and downs of pregnancy. "These are good connections after you have the baby, too," said Dr. Miller.
Learn About Postpartum Depression
You've probably heard of postpartum depression, but you may not know that 10 percent to 20 percent of women experience symptoms of major depression during pregnancy, according to the March of Dimes. This could increase your risk for preterm labor. If you're feeling unexplainably sad, angry, or guilty – or if you lose interest in activities you usually enjoy or sleep too much – tell your doctor. Therapy, a support group, an antidepressant medication, or a combination of the three will likely help. Not all antidepressants are safe for pregnant women, so be sure to work with a doctor who is familiar with pregnancy-related mental health issues. To search for a prenatal/postpartum support organization in your area, visit postpartum.net.

MD - Allopathy Gynaecological Endoscopy Specialist Infertility Specialist 12 Years Experience, Pune
Wear Sunscreen
Being pregnant makes your skin more sensitive to sunlight, so you're more prone to sunburn and chloasma, those dark, blotchy spots that sometimes appear on the face. Apply a sunscreen with an SPF of 30 or higher (many brands now offer chemical-free formulas) and wear a hat and sunglasses. While no studies prove spending time in tanning beds can hurt your baby, the American Pregnancy Association recommends you avoid them while you're pregnant.
Stay Clean
Frequent hand washing can protect you from infections such as Group B streptococcus, Fifth disease, cytomegalovirus, and chickenpox, all of which can cause birth defects and other severe complications for your baby. Ethyl alcohol-based hand sanitizers are a great option for those times when you can't get to a sink. "They protect users from most of the communicable infections," says Anjan Chaudhury, M.D., an Ob-Gyn at St. Elizabeth's Medical Center in Boston.
Travel Smart
Go ahead: book that flight, but take some precautions. The Mayo Clinic say mid-pregnancy (14 to 28 weeks) is usually the best time to fly—by this time you're probably over morning sickness, and the risk of miscarriage or early delivery is low. Still, check with your doctor about any travel plans, and make sure the airline has no restrictions for pregnant women. On the plane, drink plenty of water to stay hydrated, and get up and walk around every half hour to reduce the risk of blood clots. An aisle seat will give you more room and make trips to the bathroom easier.
In the car, continue to wear a safety belt. According to the National Highway Traffic Safety Administration, the shoulder portion of the restraint should be positioned over the collar bone. The lap portion should be placed under the abdomen as low as possible on the hips and across the upper thighs, never above the abdomen. Also, pregnant women should sit as far from the air bag as possible.